Abstract
Background: Endovascular therapy is the new standard of care for certain patients with acute ischemic stroke. We aimed to determine whether procedural volumes at an academic health sciences centre in northeastern Ontario exceeded the minimum of 20 procedures annually to support establishment of an endovascular therapy centre and thus improve regional access to this type of care.
Methods: We conducted a retrospective chart review at Health Sciences North, a regional stroke centre for northeastern Ontario that currently does not offer endovascular therapy for patients with acute ischemic stroke. Medical records and neurovascular imaging results for patients with a discharge diagnosis of cerebral infarction who were seen by the stroke on-call team at Health Sciences North between May 1, 2016, and Apr. 30, 2017, were retrospectively examined in accordance with criteria of the ESCAPE trial to identify potential candidates for endovascular therapy. The number of candidates was extrapolated to include patients discharged with cerebral infarction from referral centres within a 2-hour transport radius from the study institution.
Results: Of 71 patients who met the inclusion criteria, 9 were identified as candidates. Of the 71 cases reviewed, 62 (87%) presented within the window for administration of recombinant tissue plasminogen activator of 4.5 hours from symptom onset, 66 (93%) within the endovascular therapy window of 6 hours and 69 (97%) within the extended endovascular therapy window of 12 hours. Expanding these estimates to include regional referral centres, we conservatively estimated that Health Sciences North has the potential to perform 22 or 23 procedures annually.
Interpretation: The projected annual number of procedures met the minimum requirement to maintain competency. Establishing Health Sciences North as a centre for endovascular therapy could be an important step in improving equity in stroke outcomes across northeastern Ontario.
Five large, randomized, multicentre studies have shown the efficacy of endovascular therapy in improving functional outcomes among patients with acute ischemic stroke secondary to occlusion of a large proximal intracerebral artery.1–5 A review and meta-analysis of these trials found a significantly greater rate of functional independence at 90 days among those who received endovascular therapy than among those who received medical management alone, as indicated by a number needed to treat of 2.6 for reduction in disability level by 1 point on the modified Rankin scale.6 Endovascular therapy involves the retrieval of an intracerebral thrombus by means of a retrieval stent or thrombus aspiration device.7 Despite being resource-intensive, endovascular therapy has been found to be cost-effective.8 Of the 5 randomized trials, the ESCAPE trial showed the greatest improvement in functional outcomes and the greatest reduction in mortality among those receiving endovascular therapy, relative to medical management alone.2
Currently, Ontario has 10 health sciences centres that offer endovascular therapy, most of which are clustered in southern Ontario. Health Sciences North is a regional stroke centre for northeastern Ontario, accepting patients with hyperacute stroke from the district through an emergency medical services bypass protocol. It has access to advanced neuroimaging, fellowship-trained neuroradiologists, and acute stroke and rehabilitation units, but it currently does not offer endovascular therapy; as a result, candidates for such therapy must be transported to an existing centre. Current standards for emergency medical services dictate that transport time from a referral centre to an endovascular therapy centre by land or air ambulance should not exceed 2 hours.9 Health Sciences North is outside this maximum transport time, which largely prevents eligible patients from accessing care. The CorHealth Ontario endovascular therapy steering committee has suggested that centres outside the transport time start capacity planning to establish new centres.9 However, current Health Quality Ontario guidelines (published in 2016) suggest that an endovascular therapy centre must perform a minimum of 20 procedures annually to maintain competency,9 in accordance with guidelines set out by the World Federation of Interventional and Therapeutic Neuroradiology and adopted by the American Society of Neuroradiology, the Canadian Interventional Neuroradiology Group and the Canadian Society of Neuroradiology.10
Our objective was to determine whether the number of potential candidates for endovascular therapy presenting to Health Sciences North exceeds the minimum number of 20 cases per year to support establishment of an endovascular therapy centre. We predicted that the candidate volume, once projected to include referring centres within northeastern Ontario, would meet the minimum value of 20 annual procedures.
Methods
Study design and patient population
We determined the number of potential candidates through a retrospective chart review of all patients with a discharge diagnosis of cerebral infarction who were admitted to Health Sciences North between May 1, 2016, and Apr. 30, 2017. This study design accounted for current stroke protocol practices at Health Sciences North. This design helps to identify protocol changes that will be required to support an endovascular therapy program. The study design was partially based on a study by Rai and associates,11 who also used a retrospective methodology and extrapolation to other centres.
Men and women over 18 years of age were eligible. We included in the review only patients who presented within 24 hours after symptom onset and were seen by the stroke on-call team, which consults for thrombolysis eligibility. Patients not seen by the stroke on-call team do not undergo arch-to-vertex computed tomography (CT) angiography upon presentation, which was required to assess eligibility. We also included patients who either went directly to Health Sciences North through emergency medical services bypass or presented to an emergency department in Health Sciences North’s catchment area and were subsequently transferred to Health Sciences North. The bypass protocol allows emergency medical services to bypass a community hospital in Health Sciences North’s catchment area and take a patient directly to Health Sciences North if the patient meets protocol criteria.
Data collection
We obtained information about patients with a discharge diagnosis of cerebral infarction from Health Sciences North in the study period through the Discharge Abstract Database maintained by the Canadian Institute for Health Information. We also obtained discharge ischemic stroke volumes for centres within a 2-hour transport time using data collected by ICES.12 We reviewed each chart to determine clinical and imaging candidacy for endovascular therapy in accordance with the ESCAPE trial criteria13 (Appendix 1, available at www.cmajopen.ca/content/6/4/E671/suppl/DC1). We collected data from the patient’s paper chart and electronic medical records. A single person (B.L.) extracted clinical data from the emergency department record and electronic medical records. We recorded the following data: date and time of symptom onset, time of presentation (hospital arrival) to Health Sciences North’s emergency department and time of assessment by the stroke on-call team. The date and time of relevant imaging, including noncontrast CT of the head and multiphasic arch-to-vertex CT angiography, were also noted. We also recorded the patient’s score on the National Institutes of Health Stroke Scale (NIHSS).14 Modified Barthel index scores15 were not available, so we determined pre-event functional status through review of occupational therapy assessments. Patients were considered independent if they could complete activities of daily living independently. Other relevant clinical data that we collected included whether the patient arrived at the hospital via the bypass protocol and whether alteplase had been administered. Whenever possible, we cross-validated the data between the paper chart and electronic medical records.
A single staff neuroradiologist (J.G.) at Health Sciences North extracted imaging data from the non–contrast-enhanced CT of the head and multiphasic arch-to-vertex CT angiography. We calculated the ASPECTS (Alberta Stroke Programme Early CT Score),16 using unenhanced CT scans, to estimate the size of the infarct core. We determined the site of occlusion and the quality of collateral circulation from multiphasic CT angiography, which was also used to determine the feasibility of arterial access on the basis of vessel tortuosity, diameter and stenosis.
Statistical analysis
The clinical and imaging data were reviewed independently by a staff internist (P.P.) and a staff neuroradiologist (J.G.), respectively, at Health Sciences North. Candidacy for endovascular therapy was determined by the inclusion and exclusion criteria as outlined in Appendix 1. Only candidates who were independently determined to qualify for endovascular therapy both clinically and according to imaging results were considered to be candidates. If sufficient data were available, we calculated the modified Rankin score17 at 90 days after the stroke for these identified candidates, to track functional outcomes. We extrapolated the candidate rate on the basis of population and acute ischemic stroke discharges to include centres within a 2-hour transport radius to Health Sciences North, all of which are also more than 2 hours from the nearest endovascular therapy centre. Over the study period, there were a total of 553 discharges for acute ischemic stroke from Health Sciences North and all centres within a 2-hour transport time. As such, to achieve the minimum requirement of 20 procedures annually, the theoretical candidate rate that had to be exceeded was 3.6% of acute ischemic strokes.
Ethics approval
The study protocol was approved by the Research Ethics Board of Health Sciences North (REB no. 17–044).
Results
During the study period, 214 patients were discharged from Health Sciences North with a diagnosis of cerebral infarction. Of these, 143 were excluded: 9 who presented more than 24 hours after stroke onset and 134 who were not seen by the stroke on-call team. A total of 71 patient charts were included in the review.
Relevant demographic and clinical data for the 71 admissions that we reviewed are presented in Table 1. Of these 71 patients, 62 (87%) presented within the window for administration of recombinant tissue plasminogen activator of 4.5 hours from symptom onset, 66 (93%) within the window for endovascular therapy of 6 hours and 69 (97%) within the window for extended endovascular therapy of 12 hours. Imaging data are summarized in Table 2.
Demographic and clinical characteristics for patients who presented to the emergency department at Health Sciences North with ischemic stroke symptoms between May 1, 2016, and Apr. 30, 2017*
Imaging data for patients with symptoms of ischemic stroke*
Twenty-two of the patients were identified as candidates for endovascular therapy on the basis of clinical data and 11 on the basis of imaging data. Of the 49 noncandidates according to clinical data, 43 (88%) were excluded because the NIHSS score was below 5, indicating a mild stroke, or because the NIHSS score was not recorded (Table 3). Of the 60 patients who did not meet the imaging criteria for endovascular therapy, 20 (33%) were considered non-evaluable because CT angiography was not performed upon presentation (Table 4). Only 3 (15%) of these patients did not undergo CT angiography because of dye allergy or elevated creatinine. For another 36 (60%) of the patients eliminated on the basis of imaging data, CT angiography showed absence of proximal-vessel occlusion.
Candidacy for endovascular therapy on the basis of clinical factors, for patients with acute ischemic stroke presenting within 24 h of symptom onset*
Candidacy for endovascular therapy on the basis of imaging results, for patients with acute ischemic stroke presenting within 24 h of symptom onset*
Overall, 9 patients met both sets of criteria (Table 5). The 2 imaging candidates who did not meet clinical eligibility criteria were eliminated because the NIHSS score was low. The location of vessel occlusions for the 9 identified candidates is shown in Table 5.
Candidacy for endovascular therapy on the basis of clinical and imaging data combined, for patients with acute ischemic stroke presenting within 24 h of symptom onset*
Of the 9 candidates for endovascular therapy that we identified, 5 had died by 90 days after the stroke, and a modified Rankin score of 6 was assigned. Three of the candidates were lost to follow-up. The remaining candidate was assigned a modified Rankin score of 3 at 90 days, indicating moderate disability.
Incidence projections
Using the number of endovascular therapy candidates identified over the study period, we calculated the annual incidence rate of endovascular therapy candidates presenting to Health Sciences North by 2 methods: first, with the population of Health Sciences North’s catchment area and then with the number of ischemic stroke discharges from Health Sciences North over the study period.
Health Sciences North’s catchment area, which includes Greater Sudbury, Manitoulin Island, Espanola and Elliot Lake, has a population of roughly 203 700. Given our finding that 9 patients were suitable for endovascular therapy, this translates to an annual rate of ischemic strokes that would qualify for endovascular therapy of 4.42 per 100 000 person-years. In relation to the metric of ischemic stroke discharges, there were 9 endovascular therapy candidates out of 214 patients with ischemic stroke over the study period, or 4.2% of ischemic stroke cases. To predict the number of procedures likely to be performed annually, the estimate must be expanded to include regional referral centres. Given that roughly 509 000 people currently reside in northeastern Ontario, and given the estimated incidence of 4.42 candidates for endovascular therapy per 100 000 person-years, this translates to 22.50 candidates per year in this region overall.
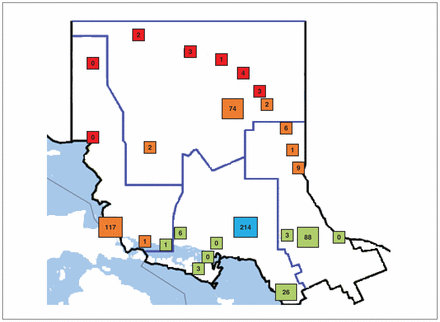
Northeastern Ontario covers more than 266 000 km2, and not all of its residents are within the 2-hour transport window to Health Sciences North by either air or land ambulance. Therefore, we also calculated the projected number of endovascular therapy candidates on the basis of number of ischemic stroke discharges from referring centres within a 2-hour transport radius to Health Sciences North. The geographic distribution of these centres, along with their ischemic stroke volumes, is shown in Figure 1. These 17 centres within a 2-hour transport time discharged 339 patients with ischemic stroke in 2016.12 Assuming that 4.2% of these patients would qualify for endovascular therapy, there would be 14.24 candidates for endovascular therapy from these centres. Including the 9 candidates that we identified at Health Sciences North, the total number of endovascular therapy candidates calculated with this alternative method is 23.24 per year. In addition, 7 community hospitals in northeastern Ontario had a total of 13 ischemic stroke discharges;12 however, these hospitals are outside the 2-hour transport time to Health Sciences North, and would represent only 0.55 missed case per year.
Distribution of hospitals and health centres in northeastern Ontario. Each hospital or health centre is represented by a coloured square. The number inside the square represents the number of discharges from that institution in 2016 for patients with ischemic stroke. The blue square represents Health Sciences North. Green squares represent centres within a 2-hour transport radius to Health Sciences North by land ambulance. Orange squares represent centres within a 2-hour transport radius to Health Sciences North by air ambulance. Red squares represent centres outside the 2-hour transport time to Health Sciences North by air or land ambulance. The 5 larger squares, including Health Sciences North, represent centres with computed tomography angiography capabilities that administer tissue plasminogen activator. Air ambulance transport times were determined in consultation with Paramedic Services for the City of Greater Sudbury. Not pictured: Cochrane-James Bay district, which had 1 ischemic stroke discharge from the Weeneebayko Area Health Authority in 2016.
Interpretation
In this retrospective study, we identified 9 patients (4.2% of the study population) at Health Sciences North who would have qualified for endovascular therapy on the basis of both clinical and imaging criteria. Extending this estimate to encompass other centres within northeastern Ontario generated estimates of 22 or 23 candidates per year, depending on whether the calculation was based on population or number of discharges after ischemic stroke. This projection exceeds the theoretical rate of 3.6% and the minimum requirement of 20 procedures per year to support the establishment of Health Sciences North as a centre for endovascular therapy.9
Compared with other population-based estimates of the incidence of patients eligible for endovascular therapy, our numbers are fairly conservative. Rai and associates11 found an incidence of 10 to 14 patients with ischemic stroke who were eligible for endovascular therapy per 100 000 person-years discharged from a tertiary-level hospital in West Virginia with a catchment population of 210 000. Similarly, Chia and colleagues18 found 11 to 22 candidates per 100 000 person-years, or 7% of admissions for acute ischemic stroke, at a hospital in Australia with a catchment population of 148 027. Despite having similar catchment population sizes and numbers of ischemic stroke discharges to Health Sciences North, both of these studies yielded estimates far higher than our projection of 4.42 candidates per 100 000 person-years.
The importance of improving access to endovascular therapy in northeastern Ontario is underscored by the poor functional outcomes of the candidates identified in our study. These poor outcomes could have been mitigated had these patients had adequate access to endovascular therapy. Several large, multicentre studies found that endovascular therapy was effective in reducing disability after stroke,1–5 with a number needed to treat of 2.6 for reduction in level of disability by 1 point on the modified Rankin scale.6
Limitations
This chart review was retrospective, so the relevant data needed to determine clinical and imaging candidacy were not always available. This limitation may have led us to miss several cases. Only one person extracted the clinical data, and another the imaging data, which decreased reliability. For several reasons, the numbers generated in our study are conservative. We used restrictive inclusion criteria to determine which patient charts would be reviewed for candidacy. Only patients seen by the stroke on-call team, which consults for thrombolysis eligibility, were included; as such, we may have excluded patients presenting more than 4.5 hours after stroke onset who might have been eligible for endovascular therapy. 14 Recently, the DAWN trial showed improvement in functional outcomes among patients receiving endovascular therapy, relative to medical management alone, who presented up to 24 hours after symptom onset.19 This finding could lead to another paradigm shift in stroke care, further increasing the potential number of candidates for endovascular therapy. We considered only patients who presented up to 12 hours after symptom onset, yet it is likely that as new data emerge, a greater proportion of patients with acute ischemic stroke will be considered eligible for endovascular therapy, and procedural volumes will increase. Indeed, a study of endovascular therapy volumes in Catalonia found a significant increase in the number of mechanical thrombectomies performed between 2011 and 2015, as more data emerged.20 Furthermore, 20 of 71 patient images reviewed in the current study were deemed non-evaluable because arch-to-vertex CT angiography was not completed upon presentation. It is possible that additional candidates would have been identified had the requisite imaging been completed. Finally, the criteria used to determine eligibility were fairly restrictive and did not allow for clinical judgment. Current recommendations of the American Heart Association indicate that endovascular therapy may be reasonable for carefully selected patients with M2 or M3 segment, anterior, posterior or vertebral artery occlusions or those with ASPECTS and/or NIHSS scores below 6.21 As such, it is likely that clinical judgment will play a role in selecting patients for endovascular therapy whose characteristics do not match the restrictive criteria f the ESCAPE trial.12 This consideration would also extend to patients with Barthel index scores below 90.
Conclusion
In this study, 9 of 71 patients admitted for acute ischemic stroke over a 12-month period met clinical and imaging criteria to qualify for endovascular therapy. Extending this projection to include major referral centres in northeastern Ontario, we conservatively estimated that Health Sciences North could perform 22 or 23 procedures per year, which exceeds the recommended annual minimum of 20 procedures set by the CorHealth Ontario endovascular therapy steering committee. Northeastern Ontario’s more than 500 000 residents currently have limited access to this new standard of care. Establishing Health Sciences North as a centre for endovascular therapy could improve functional outcomes among patients with acute ischemic stroke involving occlusion of a large proximal vessel. Bringing endovascular therapy to Health Sciences North is an essential step in ensuring equitable stroke care for the residents of northeastern Ontario.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
Contributors: Brian Lauzon was responsible for acquisition, analysis and interpretation of the data. Cathy Corrigan-Lauzon contributed to study design, oversight of data acquisition and analysis. Jonathan Grynspan contributed to study design, data acquisition and data analysis. Susan Bursey was responsible for study design. Timo Krings contributed to study design, data analysis and data interpretation. Padma Puranam contributed to data analysis and interpretation. All of the authors contributed intellectually meaningful content to drafting of the manuscript. All of the authors gave approval of the version to be published and agreed to be accountable for all aspects of the work.
Funding: This study was funded by the Local Educational Group– Hospitalist Service of the Health Sciences North Stroke Program.
Supplemental information: For reviewer comments and the original submission of this manuscript, please see www.cmajopen.ca/content/6/4/E671/suppl/DC1.
References
- Copyright 2018, Joule Inc. or its licensors