Abstract
Background: Older adults face greater risk of social isolation, but the extent of social isolation among low-income older adults living in social housing is unknown. This study aims to explore the rate of, and risk factors contributing to, subjective social isolation or loneliness among older adults in social housing.
Methods: We conducted a cross-sectional study of data collected from a community program held in the common rooms of 55 social housing buildings in 14 communities across Ontario, Canada, from May 2018 to April 2019. Participants were program attendees aged 55 years and older who resided in the buildings. Program implementers assessed social isolation using the 3-Item Loneliness Scale from the University of California, Los Angeles and risk factors using common primary care screening tools. We extracted data for this study from the program database. We compared the rate of social isolation to Canadian Community Health Survey data using a 1-sample χ2 test, and evaluated associations between risk factors and social isolation using univariate and multivariate logistic regressions.
Results: We included 806 residents in 30 buildings for older adults and 25 mixed-tenant buildings. Based on the 3-Item UCLA Loneliness Scale, 161 (20.0%) of the 806 participants were socially isolated. For those aged 65 and older, the rate of social isolation was nearly twice that observed in the same age group of the general population (36.1% v. 19.6%; p < 0.001). Risk factors were age (65–84 yr v. 55–64 yr adjusted odds ratio [OR] 1.99, 95% confidence interval [CI] 1.01–3.93), alcohol consumption (adjusted OR 2.45, 95% CI 1.09–5.54), anxiety or depression (adjusted OR 6.05, 95% CI 3.65–10.03) and income insecurity (adjusted OR 2.10, 95% CI 1.24–3.53). Protective factors were having at least 1 chronic cardiometabolic disease (adjusted OR 0.44, 95% CI 0.24–0.80), being physically active (adjusted OR 0.47, 95% CI 0.30–0.73) and having good to excellent general health (adjusted OR 0.60, 95% CI 0.39–0.90).
Interpretation: The high rate of social isolation in low-income older adults living in social housing compared with the general population is concerning. Structural barriers could prevent engagement in social activities or maintenance of social support, especially for older adults with income insecurity and anxiety or depression; interventions are needed to reduce subjective social isolation in this population.
Adults aged 65 and older are the fastest growing age group in Ontario, projected to increase from 16.9% of the population in 2018 to 23.4% by 2046.1 About 75 000 older adults live in social housing in Ontario (i.e., subsidized, rent-geared-to-income units), with 50 295 older adult households on wait lists for social housing in 2015, representing a third of households on such wait lists in Ontario.2 Social housing rental units are typically subsidized such that rent is 30% of household income, and eligibility is determined upon a complete financial assessment. Given the substantial and increasing number of older adults in Ontario living in social housing, it is relevant for stakeholders to understand factors influencing their health, such as social isolation.
Social isolation can be objectively defined as a lack of social contacts or limitation in the frequency of interaction with social network members, including family, friends and the larger community environment.3–6 Loneliness is the subjective or psychological embodiment of social isolation3–7 and will be the focus of the current study. In Canada, older adults are at high risk of subjective social isolation,7,8 with 19.6% of adults aged 65 and older reporting a lack of companionship, feeling left out or feeling isolated from others. 7,8 Older adults are particularly vulnerable given their decreasing economic resources, reduced social networks, changes in household structure and limitations in function and mobility.9
Subjective social isolation (i.e., loneliness) has been associated with living alone10 and poor health behaviours, such as smoking3 and physical inactivity.11,12 It has also been associated with an increased risk of cardiovascular disease, stroke, depression, dementia and all-cause death.5,13–15 These health outcomes are particularly important for older adults living in social housing, given that this population reports poorer health and faces higher mortality rates than their unsubsidized counterparts.16,17 Subjective social isolation also affects the broader community by increasing the use of health and social services.18 For example, older adults with subjective social isolation have higher rates of certain high-cost and possibly avoidable health care services, such as hospital readmissions and long hospitalizations.19
Although low income has been associated with subjective social isolation in the general population, few studies have focused on social isolation in low-income older adults,20,21 and we could not identify any quantitative studies with older adults in social housing. We identified only 1 qualitative study of low-income older adults living in social housing, which found that they typically have less social support and therefore face an even greater risk of social isolation.22 By identifying risk factors in this population, targeted interventions and policies could be developed to prevent social isolation and thereby improve quality of life,17 reduce health inequalities19 and decrease health system costs associated with social isolation in an aging population.19 Given the gap in literature on this hard-to-reach population, we aimed to explore the rate of, and risk factors contributing to, social isolation in low-income older adults in social housing. We hypothesized that older adults living in social housing in Ontario would have higher rates of social isolation compared with the general population.
Methods
Setting
We conducted this cross-sectional study with data from the Community Paramedicine at Clinic (CP@clinic) program. CP@clinic is a voluntary, community-based program for health promotion and disease prevention that considers a holistic approach to health. It is held weekly in social housing for older adults. The program is advertised via posters throughout the building, encouraging residents to drop into sessions as a way to have a health check to prevent impending health issues. Paramedics hold sessions, conduct validated health-risk assessments through 1-on-1 clinical questioning, provide tailored health education and offer referrals to community resources on the basis of the results. The paramedics and CP@clinic program staff fax assessment results to the participant’s family physician, with consent. The program is offered in social housing buildings for a 6-to-12-month period at a time. We have previously published a detailed description of CP@clinic.23
Participants
In accordance with the definition of “senior” used to determine housing eligibility by many Ontario Housing providers, we defined older adults as those aged 55 years and older.23 Study participants were older adults living in 55 designated social housing buildings for older adults or mixed tenants receiving the CP@clinic program. Buildings were in 14 regions across Ontario, Canada (i.e., Frontenac County, Grey County, Guelph, Halton Region, Hamilton, Hastings Region, Hearst, Iroquois Falls, Matheson, Norfolk Region, Peel Region, Sudbury, Timmins and York Region). Participants must have attended the program. The buildings designated for older adults had only tenants determined to be older adults according to the local housing authority’s criteria; mixed-tenant buildings had residents of other ages as well.
Data collection and measures
We collected data between May 2018 and April 2019. After receiving participant consent, paramedics collected their data as part of the health-risk assessment screening during the course of an individual CP@clinic session; validated tools were used to reduce response bias.4,24–26 Paramedics entered data into the CP@clinic database, which is an electronic medical record (EMR). Paramedics are trained to use the assessments; additionally, day-to-day paramedic work now encompasses community paramedicine, which includes wellness check clinics (see Appendix 1, available at www.cmajopen.ca/content/9/3/E915/suppl/DC1, for the subset of fields from the EMR included in this study).
We measured subjective social isolation using the validated University of California, Los Angeles (UCLA) 3-Item Loneliness Scale. This scale was already embedded within the EMR to measure subjective social isolation as it is a recommended primary care screening tool27 and has also been used by Statistics Canada.7 It assesses the participant’s own perception of their loneliness, which differs from objective measures of social contacts.4 Participants answered the following 3 questions: “How often do you feel that you lack companionship?”, “How often do you feel left out?” and “How often do you feel isolated from others?”. The response options were “hardly ever,” “some of the time” or “often,” which corresponded to a score of 1, 2 or 3, respectively. The final score was the sum of all items, for a minimum score of 3 and maximum of 9. We considered a participant with a score 6 or over as socially isolated in accordance with the guidance of the Centre for Addiction and Mental Health.27,28 The 2008–2009 Canadian Community Health Survey (CCHS) Healthy Aging Module also used this set of questions,7 which allowed us to compare our sample and the general population for people aged 65 and older. For the purpose of this comparison only, we used a score of 5 and over to define subjective social isolation, matching the cut-off used by the CCHS.7
We extracted risk factors from the CP@clinic EMR. Sociodemographic data included age, gender, ethnicity, marital status and living alone. Physical measures included weight, height and body mass index (BMI). In addition, participants self-reported their chronic cardiometabolic disease history (i.e., transient ischemic attack or stroke, heart attack, hypertension, hyperlipidemia and diabetes). We collected information on physical activity,11,12,24 alcohol use (any alcohol consumption v. nondrinker),29,30 current smoking status (current smoker v. former or never),3,31 income security11,25 and self-reported general health,11,26 based on literature associating these factors with social isolation. We measured health-related quality of life using 5 domains from the EQ-5D-3L tool, namely mobility, self-care, usual activities, pain or discomfort, and anxiety or depression.32,33
Statistical analysis
We performed descriptive statistics. For participants aged 65 and older, we used a 1-sample χ2 test to compare subjective social isolation in the study sample to the fixed value reported by the 2008–2009 CCHS for the same age category.
For the full study sample (aged 55 and older), we used univariate binary logistic regression models to analyze associations for each independent variable (i.e., sociodemographic factors and health-related indicators) with social isolation. We used multivariable logistic regression models to evaluate the association of all independent variables with social isolation concurrently for participants with complete cases. We also replicated all regression models for the “lives alone” and “does not live alone” subgroups. To limit the number of variables in the regression models and to account for response options with small numbers, we collapsed some variables into fewer response categories (e.g., ethnicity, BMI categories, alcohol consumption, smoking status, presence of at least 1 chronic cardiometabolic disease). Some variables were also not included in the final model because of their very high correlation with another independent variable (e.g., marital status and living alone). We conducted model diagnostics to evaluate collinearity.
We verified data to complete the cases with missing gender at intake. We completed all analyses with IBM SPSS Statistics 17.0.
Ethics approval
This study was approved by the Hamilton Integrated Research Ethics Board (no. 14-645).
Results
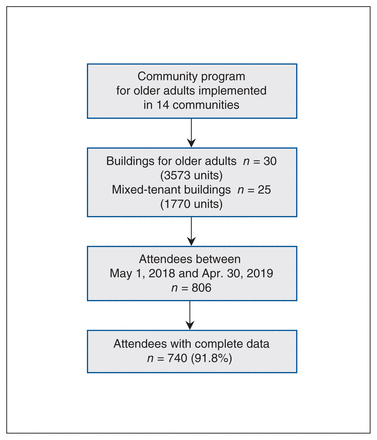
The study included all 806 residents who attended the CP@clinic program in 30 buildings for older adults (3573 apartment units) and 25 mixed-tenant buildings (1770 apartment or townhouse units) (Figure 1). The 806 participants were most commonly female (n = 609, 75.6%), aged 65–84 years (n = 517, 64.1%), white (n = 603, 74.8%) and widowed (n = 310, 38.5%). Most lived alone (n = 625, 77.5%), had some high school education or less (n = 357, 44.3%) and had a family doctor (n = 722, 89.6%).
Participant flow diagram.
One in 5 (20.0%) participants were classified as having social isolation (Table 1). Similarly, for participants aged 65 and older, 20.7% were classified as having social isolation. Complete data were available for 740 participants (91.8%). Among the 161 participants classified as having social isolation, a high proportion were current smokers (n = 40, 24.8%), were income insecure (n = 47, 29.2%) and had anxiety or depression (n = 114, 70.8%), as well as having poor to fair health (n = 74, 46.0%), a history of stroke or transient ischemic attack (n = 32, 19.9%), and diabetes (n = 63, 39.1%).
Sociodemographic factors, health behaviours and health-related quality of life for all study participants and by social isolation subgroup
We compared the study sample to the general population in the 2008/09 CCHS Healthy Aging survey by matching the CCHS cut-off score of 5 on the UCLA 3-item Loneliness Scale and restricting the study sample to only those aged 65 and older. The rate of social isolation or loneliness among low-income older adults living in social housing was significantly higher than in the general population (36.1% v. 19.6%, χ2 = 72.8, df = 1, p < 0.001).
The univariate regressions found significant factors associated with increased odds of social isolation, including living alone, low physical activity, alcohol consumption, smoking, poor to fair general health, mobility problems, self-care problems, problems doing usual activities, pain or discomfort, anxiety or depression and income insecurity (Table 2). When all factors were analyzed together in a multivariable regression, we did not identify any issues with multicollinearity (variance inflation factors 1.03–1.64). Significant risk factors for social isolation in the multivariable model were age (65–84 yr v. 55–64 yr adjusted odds ratio [OR] 1.00, 95% confidence interval [CI] 1.01–3.93), alcohol consumption (adjusted OR 2.45, 95% CI 1.09–5.54), anxiety or depression (adjusted OR 6.05, 95% CI 3.65–10.03) and income insecurity (adjusted OR 2.10, 95% CI 1.24–3.53). Protective factors were having at least 1 chronic cardiometabolic disease (adjusted OR 0.44, 95% CI 0.24–0.80), being physically active (adjusted OR 0.47, 95% CI 0.30–0.73) and having good to excellent general health (adjusted OR 0.60, 95% CI 0.39–0.94).
Univariate and multivariable binomial logistic regression of having self-reported social isolation*
Of the 625 participants who lived alone, 136 (21.8%) reported social isolation. Univariate regressions found significant factors associated with increased odds of social isolation for this subgroup, including being female, age (65–84 yr v. 55–64 yr), low physical activity, alcohol consumption, smoking, having poor to fair general health, mobility problems, self-care problems, problems doing usual activities, anxiety or depression and income insecurity (Table 3). For the multivariable regression, we did not identify any multicollinearity (variance inflation factors 1.03–1.65). The multivariable regression found increased odds of social isolation with alcohol consumption (adjusted OR 3.11, 95% CI 1.27–7.63), anxiety or depression (adjusted OR 6.27, 95% CI 3.59–10.97) and income insecurity (adjusted OR 1.93, 95% CI 1.11–3.37), and decreased odds of social isolation with physical activity (adjusted OR 0.45, 95% CI 0.27–0.73).
Univariate and multivariable binomial logistic regression of having self-reported social isolation among participants who live alone*
Of the 175 participants who did not live alone, 24 (13.7%) reported social isolation. For this subgroup, univariate regressions found significantly increased odds of social isolation (p < 0.05) associated with income insecurity (OR 4.67, 95% CI 1.52–14.37), smoking (OR 10.21, 95% CI 3.27–31.89), problems doing usual activities (OR 2.43, 95% CI 1.01–5.87), and anxiety or depression (OR 4.99, 95% CI 1.77–14.07), and decreased odds of social isolation with having good to excellent general health (OR 0.37, 95% CI 0.15–0.91) (Table 4). As the number of individuals who did not live alone and were socially isolated was small, it did not support conducting a multivariable logistic regression analysis for this subgroup.
Univariate binomial logistic regression of having self-reported social isolation in participants who do not live alone*
Interpretation
Our results show that 1 in 5 low-income older adults living in social housing had subjective social isolation or loneliness. For adults aged 65 and older, the rate of social isolation observed in this sample was nearly twice that reported in the general population.7 When adjusting for all of the risk factors simultaneously, physical activity and having at least 1 chronic cardiometabolic disease were consistently protective against social isolation, and alcohol consumption, poor to fair general health, anxiety or depression and income insecurity were risk factors. Living alone was more common among those who were socially isolated than not socially isolated (84% v. 75%); however, the results of this study suggest that in a population where most people do live alone, other factors (e.g., income insecurity) may be more strongly associated with feeling socially isolated than living alone.
Within the study population, income insecurity was significantly associated with greater odds of being socially isolated. Low income can prevent individuals from engaging in social activities or limit their ability to develop and maintain social support.34 In previous studies, low-income participants identified inaccessibility of amenities and a lack of opportunities to connect with others through education and employment as key causes of social isolation.20 Lack of a vehicle or efficient public transportation often prevented lower-income individuals from accessing community activities.20 Similar structural factors likely contribute to the increased rate of social isolation in our study population. For example, the Ontario Non-Profit Housing Association reports that social housing sites, with high-rise buildings and lack of proximity to amenities, are not well-suited for the needs of older adults.35 Thus, older tenants with mobility issues or limited transportation lack accessible opportunities for social participation, with some reporting that they felt confined to their units.35,36
As the negative relationship between social isolation and health is well known,9 we might expect those with poor to fair health or who were physically inactive to be at greater odds for experiencing social isolation. Social isolation is a risk factor for negative health consequences, ranging from depression to coronary heart disease.13 These conditions may then exacerbate social isolation, as individuals with health concerns may struggle to visit friends and family or to engage in community activities. Furthermore, socially isolated individuals have been found to be less likely to exercise or consistently consume fruits and vegetables, and more likely to smoke; these negative health behaviours may worsen experiences of isolation.3 It has been theorized that social relationships benefit health primarily through encouraging health-promoting behaviours, such as exercise and adherence to therapeutic regimes, or by discouraging negative health behaviours, such as smoking.37 In addition, social ties may also connect people to social networks that facilitate access to resources supportive of health, such as medical referrals or job opportunities.38 This cycle of social isolation and health consequences may contribute to the high rate of social isolation in our study population, which has previously been reported to have poorer health outcomes and less social support.22
Finally, in keeping with our findings, living alone is associated with social isolation.10 Previous research has found that lack of social support is common among older adults who live alone, which in turn contributes to social isolation.39 Mental health problems are also more common in low-income populations, 40 and almost half of the current study sample reported having anxiety or depression. This risk factor was found to have the strongest association with social isolation in the multivariable models; however, the direction of this relation cannot be determined from this cross-sectional study. It is plausible that this is a bidirectional relation, whereby social isolation can result in anxiety and depression, and having anxiety or depression could result in being socially isolated.41 Further research is needed to understand this complex dynamic better.
The health outcomes of social isolation are particularly important to low-income older adults in social housing, given their health inequalities. Our work suggests that low-income older adults in social housing are at heightened risk of social isolation and the negative consequences that follow. Certain subgroups, such as those reporting income insecurity, are particularly vulnerable. Targeted interventions have the potential to support these individuals. For example, social prescribing is an emerging approach for addressing loneliness and social isolation.18 It involves referring individuals to community support and social programming, such as befriending schemes or group lessons.42 This approach could be very successful for lower-income older adults in social housing, as previous literature suggests they value relationships with community program providers.43 In addition, addressing social isolation in this population represents an opportunity to reduce health inequalities and health care costs. Older adults who are socially isolated are 4–5 times more likely to be hospitalized than those who are not socially isolated.44 Thus, directing support to this group could curb rising health care spending associated with an aging population.
Limitations
The current study evaluated a sample of older adults in social housing. We acknowledge that our sample may be biased by the large number of women who participated in the program. However, there are no data published on the target population in Ontario with which we can compare to assess representation. This is a substantial gap in the research literature. The cross-sectional nature of our study limits our ability to ascertain the direction of the relation between social isolation and associated factors. Also, the large number of comparisons with uncorrected p values and the small sample sizes may have resulted in type I and type II errors, respectively.
Participants may have underreported their experiences of social isolation because of a bias toward social desirability. We acknowledge that it would be difficult to administer these social isolation questions in any other way, given poor education and health literacy, as well as the nature of the population. 45 Residents of social housing may be more suspicious of unfamiliar people and hesitant to participate,41 but paramedics are viewed as trusted professionals and advocates by this population. 43 Furthermore, participants may have previously met the paramedics who collected the data, potentially contributing to self-reporting bias.
Finally, the sampling method may have increased the risk of self-selection bias. Advertisements for CP@clinic were placed around the social housing buildings, and participants chose whether they attended the program. Consequently, individuals who elected to participate may have been healthier, less socially isolated and more mobile than the general population of low-income older adults living in social housing. Nonetheless, this study provides valuable insight into a marginalized population that has not been well studied.
Conclusion
Canada’s aging population is expected to create a large number of low-income older adults living in social housing because of limited finances and increased debt when entering retirement. We found that this population has higher rates of social isolation than the general population, and is therefore at greater risk of associated negative health consequences. We found several factors associated with increased odds of being socially isolated in our study population, such as self-reported anxiety or depression and income insecurity. These findings should inform the development of interventions to support vulnerable subgroups.
Although this study’s strength is in addressing a gap in the international evidence base by assessing a hard-to-reach population, further longitudinal research is needed on the causal links between social isolation and negative health outcomes in this group. This research, and subsequent programs targeting social isolation in low-income older adults in social housing, can help improve well-being, address health inequities and reduce health care costs associated with Canada’s aging population.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
Contributors: Gina Agarwal, Melissa Pirrie, Ricardo Angeles and Francine Marzanek conceived and designed the study, and collected data. Melissa Pirrie, Angela Gao and Ricardo Angeles conducted statistical analyses. Gina Agarwal and Angela Gao drafted the manuscript, and Melissa Pirrie and Gina Agarwal participated in critical revision of the article. All authors have reviewed and gave final approval of the version to be published, and agreed to be accountable for all aspects of the work.
Funding: This study was funded by a Canadian Institutes of Health Research grant (MOP-133563).
Data sharing: Limited deidentified data can be shared by the lead author upon request.
Supplemental information: For reviewer comments and the original submission of this manuscript, please see www.cmajopen.ca/content/9/3/E915/suppl/DC1.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/
References
- © 2021 CMA Joule Inc. or its licensors