Abstract
Background Sodium–glucose cotransporter-2 (SGLT2) inhibitors are cardioprotective agents in patients with type 2 diabetes mellitus and atherosclerotic cardiovascular disease (CVD). Since little is known about their uptake in atherosclerotic CVD, we examined SGLT2 inhibitor prescribing trends and identified potential disparities in prescribing patterns.
Methods We conducted an observational study using linked population-based health data in Ontario, Canada, from April 2016 to March 2020 of patients aged 65 years or older with concomitant type 2 diabetes and atherosclerotic CVD. To examine prevalent prescribing of SGLT2 inhibitors (canagliflozin, dapagliflozin and empagliflozin), we constructed 4 cross-sectional yearly cohorts from Apr. 1 to Mar. 31 (2016/17, 2017/18, 2018/19 and 2019/20). We estimated prevalent SGLT2 inhibitor prescribing by year and by subgroups, and identified factors associated with SGTL2 inhibitor prescribing using multivariable logistic regression.
Results There were 208 303 patients in our overall cohort (median age 74.0 yr [interquartile range 68.0–80.0 yr], 132 196 [63.5%] male). Although SGLT2 inhibitor prescribing increased over time, from 7.0% to 20.1%, statin prescribing was initially 10-fold higher and later threefold higher than SGLT2 inhibitor prescribing. In 2019/20, SGLT2 inhibitor prescribing was roughly 50% lower among those aged 75 years or older than among those younger than 75 years (12.9% v. 28.3%, p < 0.001) and in women than in men (15.3% v. 22.9%, p < 0.001). Age 75 years or older, female sex, history of heart failure and kidney disease, and low income were independent factors of lower SGLT2 inhibitor prescribing. Among physician specialists, visits to endocrinologists and family physicians were stronger factors of SGLT2 inhibitor prescribing than cardiologist visits.
Interpretation We found that 1 in 5 patients with diabetes and atherosclerotic CVD were prescribed SGLT2 inhibitors in 2019/20, whereas statins were prescribed for 4 of every 5 patients. Although SGLT2 inhibitor prescribing increased over the study period, disparities in adoption by age, sex, socioeconomic status, comorbidities and physician specialty remained.
Breakthrough evidence supporting sodium–glucose cotransporter-2 (SGLT2) inhibitors as cardioprotective agents has recently transformed the management of heart disease.1–4 Although these agents were originally developed as glucose-lowering agents for people with type 2 diabetes mellitus, they were found to not only lower blood glucose levels but also reduce rates of cardiovascular events and mortality in clinical trials of patients with atherosclerotic cardiovascular disease (CVD) and type 2 diabetes.1–4 Furthermore, clinical trials showed cardiovascular benefits in patients with type 2 diabetes and kidney disease.5,6 These findings shifted the therapeutic focus from glucose lowering to cardioprotection, which led to cardiologists being introduced to the realm of type 2 diabetes. Sodium–glucose cotransporter-2 inhibitors add to the current armamentarium of cardioprotective medications of statins, angiotensin-converting-enzyme (ACE) inhibitors/angiotensin receptor blockers (ARBs), β-blockers (in selected populations) and antiplatelet agents.4,7
Much of the uptake of SGLT2 inhibitors has focused on patients with heart failure or type 2 diabetes. Early studies showed slow SGLT2 inhibitor adoption of 5%–10% in type 2 diabetes populations;8–10 however, evaluation of SGLT2 inhibitors in type 2 diabetes and atherosclerotic CVD has been limited. Given that patients with type 2 diabetes and concomitant atherosclerotic CVD have high cardiovascular risk, we focused our evaluation on SGLT2 inhibitor use in this population, who may receive more clinical benefit from SGLT2 inhibitors than those with type 2 diabetes alone. Even in high-risk groups, however, adoption of novel therapies that require a paradigm shift in thinking can be delayed. This occurred with the introduction of statins, which transitioned from lipid-lowering to cardiac risk reduction agents.11 Sodium–glucose cotransporter-2 inhibitors are now being labelled as the “new statins,” and they may face similar challenges.12 The objective of our study was to characterize the contemporary adoption of SGLT2 inhibitors in patients with concomitant diabetes and atherosclerotic CVD, and identify potential disparities in prescribing patterns. This information may assist in developing targeted interventions to improve SGLT2 inhibitor prescribing and mitigate prescribing disparities.
Methods
Study design and setting
We conducted an observational study using population-based health data in Ontario, Canada. Ontario residents aged 65 years or older receive prescription drug coverage through the Ontario Drug Benefit program. We reported the study following the Reporting of Studies Conducted Using Observational Routinely-collected Data (RECORD) statement (http://www.record-statement.org).
Data sources
We used health care databases at ICES, an independent, nonprofit research institute. We obtained data on diagnoses from the Canadian Institute for Health Information Discharge Abstract Database and the National Ambulatory Care Reporting System database, data on outpatient prescription medication from the Ontario Drug Benefit prescription claims database, procedure information from the Ontario Health Insurance Plan and Canadian Institute for Health Information databases, information on physician visits from the Ontario Health Insurance Plan, physician specialty from the ICES Physician Database, data on vital status (mortality) from the Ontario Registered Persons Database, and neighbourhood income information from Statistics Canada census data. These databases were linked by means of unique encoded identifiers and analyzed at ICES. The senior author and the research analysts had full access to all the data in the study and take responsibility for data integrity and analysis.
Study population
We included patients aged 65–105 years with diagnoses of both atherosclerotic CVD and diabetes recorded between Apr. 1, 2016, and Mar. 31, 2020. We defined atherosclerotic CVD using validated International Statistical Classification of Diseases and Related Health Problems, 10th Revision (ICD-10) codes for myocardial infarction, chronic ischemic heart disease, angina, peripheral vascular disease and cerebrovascular disease, or Canadian Classification of Health Interventions codes for percutaneous coronary intervention or coronary artery bypass grafting in the prior 10 years13 (Appendix 1, Supplemental Table S1, available at www.cmajopen.ca/content/11/3/E494/suppl/DC1). We defined diabetes according to established, validated diabetes algorithms that have been used extensively at ICES for defining diabetes.14,15 We excluded patients who were long-term care residents.
Cohort creation
To examine prevalent prescribing, we constructed 4 cross-sectional yearly cohorts from Apr. 1 to Mar. 31 (2016/17, 2017/18, 2018/19 and 2019/20). Patients with a diagnosis of atherosclerotic CVD within 10 years before Apr. 1 of the cohort year and a diagnosis of diabetes at any time before were included in that yearly cohort. For the analysis of factors associated with SGLT2 inhibitor prescribing, we constructed a merged cohort that included only unique patients from within the 4 yearly cohorts between Apr. 1, 2016, and Mar. 31, 2020, using the same inclusion and exclusion criteria.
Outcome measures
The outcomes of the study were prescribing of SGLT2 inhibitors and factors associated with SGLT2 inhibitor prescribing (Appendix 1, Supplemental Table S2). For SGLT2 inhibitor prescribing, we determined the proportion of patients who filled 1 or more SGLT2 inhibitor prescriptions within 1 year of the Apr. 1 index date of each yearly cohort. For the analysis of factors associated with SGLT2 inhibitor prescribing, we defined SGLT2 inhibitor prescribing as 1 or more SGLT2 inhibitor prescriptions dispensed within 1 year after the date of diagnosis of concomitant atherosclerotic CVD and diabetes.
Statistical analysis
We described baseline characteristics of the cohort and compared characteristics of patients who did and did not fill an SGLT2 inhibitor prescription using standardized differences. Baseline characteristics included demographic characteristics, comorbidities and cardiac procedures in the prior 10 years, medications dispensed in the prior 90 days, outpatient physician visits in the prior year and the Hospital Frailty Risk Score at the index date.16 We estimated SGLT2 inhibitor use in each yearly cohort and compared prescribing of SGLT2 inhibitors to that of commonly prescribed cardioprotective agents (statins and ACE inhibitors/ARBs) (Appendix 1, Supplemental Table S3). We also conducted several preplanned analyses, stratifying by patient age (< 75 yr v. ≥ 75 yr), sex (male v. female) and history of chronic kidney disease (CKD) (v. not), using using ICD-10 codes E10.2, E11.2, E13.2, E14.2, I12, I13, N8, N18 and N28, and by history of heart failure (v. not) using ICD code I50.
We used multivariable logistic regression models to estimate odds ratios (ORs) and 95% confidence intervals (CIs) to identify factors associated with SGLT2 inhibitor prescribing. We selected covariates for the models based on prior literature, clinical experience and expert opinion, and included baseline demographic characteristics, comorbidities, laboratory values, concomitant medications, use of health care services and year of cohort entry. We tested collinearity and considered the threshold of variance inflation factors of less than 5 for covariate removal.17 All analyses were performed with SAS version 9.4 (SAS Institute). A 2-sided p value < 0.05 was considered statistically significant.
Ethics approval
ICES’ legal status under Ontario’s Personal Health Information Protection Act allows it to collect and analyze health care and demographic data, without consent, for health system evaluation and improvement. The use of data in this project is authorized under section 45 of the Personal Health Information Protection Act and does not require review by a research ethics board. The data set from this study is held securely in coded form at ICES.
Results
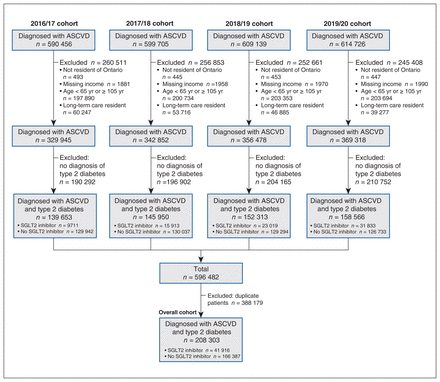
We identified 139 653, 145 950, 152 313 and 158 566 patients diagnosed with both diabetes and atherosclerotic CVD in the 2016/17, 2017/18, 2018/19 and 2019/20 cohorts, respectively (Figure 1; Appendix 1, Supplemental Table S3). There were 208 303 unique patients with a median age of 74.0 (interquartile range [IQR] 68.0–80.0) years, of whom 132 196 (63.5%) were male. In each yearly cohort, about 94.5% of patients had hypertension, 26.8%–28.5% had CKD, about 21.5% had heart failure, 73.2%–74.8% were dispensed statins, and 63.7%–66.6% were dispensed ACE inhibitors/ARBs at baseline. In all cohorts, patients who were versus were not dispensed an SGLT2 inhibitor were younger (e.g., 2019/20 cohort: median age 72.0 yr [IQR 68.0–76.0 yr] v. 76.0 yr [IQR 71.0–82.0 yr]) (p < 0.001 for each yearly comparison), had fewer comorbidities and had lower Hospital Frailty Risk Score values (e.g., 2019/20 cohort: mean 2.94 [standard deviation 4.53] v. 5.19 [standard deviation 6.99]) (p < 0.001 for each yearly comparison) (Appendix 1, Supplemental Table S2).
Flow diagram showing patient selection. Note: ASCVD = atherosclerotic cardiovascular disease, SGLT2 = sodium–glucose cotransporter-2.
Temporal patterns of prescribing of SGLT2 inhibitors and other cardioprotective medications
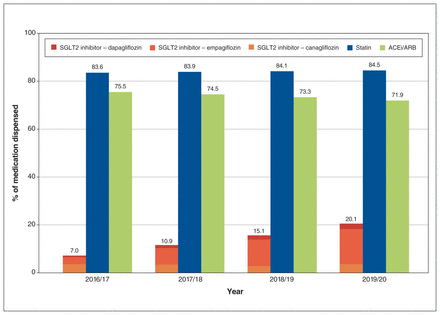
The proportion of patients dispensed an SGLT2 inhibitor within 1 year of cohort entry increased about threefold over the study period, from 7.0% in 2016/17 to 10.9% in 2017/18, 15.1% in 2018/19 and 20.1% in 2019/20. Empagliflozin accounted for an increasing proportion of SGLT2 inhibitor prescriptions, from 42.2% of patients in 2016/17 to 73.1% of patients in 2019/20. The proportion of patients dispensed a statin within 1 year of cohort entry increased negligibly over the study period, and the proportion of patients dispensed an ACE inhibitor/ARB within 1 year of cohort entry decreased slightly. In 2016/17, statin prescribing and ACE inhibitor/ARB prescribing were about 10 times that of SGLT2 inhibitors (p < 0.001), whereas in 2019/20, statin prescribing and ACE inhibitor/ARB prescribing were roughly 4 times higher than SGLT2 inhibitor prescribing (p < 0.001) (Figure 2). Empagliflozin prescribing increased 5.1-fold during the study period, dapagliflozin prescribing increased 3.1-fold, and canagliflozin prescribing did not increase.
Temporal trends of cardioprotective medication use within 1 year of cohort entry. Note: ACE = angiotensin-converting-enzyme, ARB = angiotensin II receptor blocker, SGLT2 = sodium–glucose cotransporter-2.
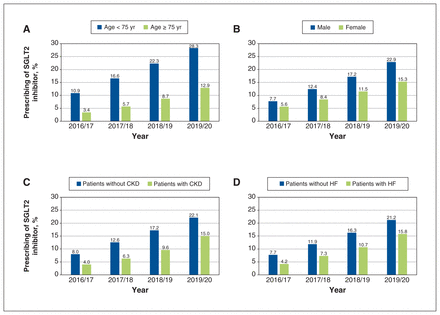
Prescribing of SGLT2 inhibitors increased in all subgroups. Patients aged 75 years or older, those with CKD and those with heart failure had the greatest relative increase, 3.8-fold, over the study period (Figure 3). In 2019/20, SGLT2 inhibitor prescribing among those aged 75 years or older was still 54.4% lower than among those younger than 75 years (12.9% v. 28.3%, p < 0.001). Prescribing of SGLT2 inhibitors was 49.7% higher in men than in women (22.9% v. 15.3%, p < 0.001), 47.3% higher in those without CKD than those with CKD (22.1% v. 15.0%, p < 0.001) and 34.2% higher in those without than with heart failure (21.2% v. 15.8%, p < 0.001). Prescribing rates varied among SGLT2 inhibitors.
Temporal trends of sodium–glucose cotransporter-2 (SGLT2) inhibitor prescribing by subgroup. Note: CKD = chronic kidney disease, HF = heart failure.
Factors associated with SGLT2 inhibitor prescribing
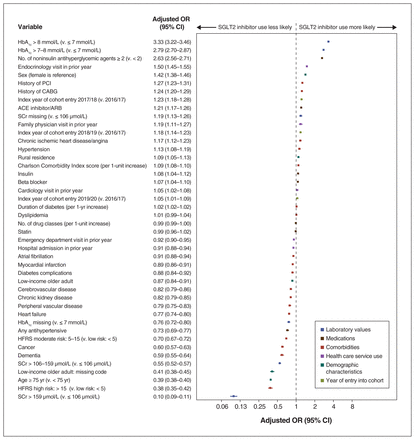
The highest variance inflation factor on collinearity testing was 2.55, which was below the threshold of less than 5. We included the 208 303 unique patients with diabetes and atherosclerotic CVD in the analysis of factors associated with SGLT2 inhibitor prescribing. Factors most strongly associated with higher SGLT2 inhibitor prescribing included glycated hemoglobin concentration greater than 8 mmol/L versus 7 mmol/L or less (OR 3.33, 95% CI 3.22–3.46), prescribing of 2 or more non-insulin antihyperglycemic agents (OR 2.63, 95% CI 2.56–2.71), an endocrinologist visit in the prior year (OR 1.50, 95% CI 1.45–1.55) and male sex (OR 1.42, 95% CI 1.38–1.46) (Table 1, Figure 4). Age 75 years or older (OR 0.39, 95% CI 0.38–0.40), a history of heart failure (OR 0.77, 95% CI 0.74–0.80), an elevated serum creatinine level (> 106–159 μmol/L v. ≤ 106 μmol/L) (OR 0.55, 95% CI 0.52–0.57) and low annual income (< $19 300) (OR 0.87, 95% CI 0.84–0.91) were some of the factors associated with lower odds of SGLT2 inhibitor prescribing.
Baseline characteristics of the cohort by SGLT2 inhibitor prescribing
Factors associated with sodium–glucose cotransporter-2 (SGLT2) inhibitor prescribing within 1 year of concomitant diagnosis of diabetes mellitus and atherosclerotic cardiovascular disease. Note: ACE = angiotensin-converting-enzyme, ARB = angiotensin II receptor blocker, CABG = coronary artery bypass graft surgery, CI = confidence interval, CKD = chronic kidney disease, HbA1c = glycated hemoglobin, HFRS = Hospital Frailty Risk Score, OR = odds ratio, PCI = percutaneous coronary intervention, SCr = serum creatinine.
Interpretation
In a contemporary, real-world population of patients with diabetes and atherosclerotic CVD, we found limited prescribing of SGLT2 inhibitors and identified important factors associated with SGLT2 inhibitor prescribing. Although prescribing increased over time, in the most recent year (2019/20), only 1 in 5 patients was dispensed an SGLT2 inhibitor within 1 year of being identified as having both diseases. Furthermore, prescribing of SGLT2 inhibitors was far lower than that of other common secondary prevention agents, such as statins and ACE inhibitors/ARBs. Although the greatest increase in SGLT2 inhibitor prescribing over the study period was observed among patients aged 75 years or older, and those with concomitant CKD and heart failure, prescribing remained well below that among younger patients and those without those comorbidities. Markers of worse glycemic control, including endocrinologist visits, in patients with diabetes were associated with higher odds of SGLT2 inhibitor prescribing, and comorbidities, female sex, older age and socioeconomic disparities were associated with lower odds of prescribing. Although a cardiologist visit in the prior year was associated with SGLT2 inhibitor prescribing, the relative odds were far below that for an endocrinologist visit.
We found that SGLT2 inhibitor prescribing increased threefold over the study period, from 7% to 20%. However, previous studies in atherosclerotic CVD and diabetes populations showed lower rates of SGLT2 inhibitor adoption.8,10 Studies using commercially insured databases in the United States showed increasing rates of SGLT2 inhibitor prescribing — from 3% in 2015 to 10% in 20198,10 — that are about 50% lower than our study rates. Although prior authorization and high cost have been identified as barriers to SGLT2 inhibitor uptake in the US,18 these barriers did not affect our study population, as prior authorization policies are not imposed for SGLT2 inhibitors in this setting, and SGLT2 inhibitors are covered on the provincial formulary without additional patient copay beyond usual rates (typically $2.00–$6.11 for any prescription dispensed). Therefore, the higher rates of SGLT2 inhibitor adoption observed in our study may have been related to the absence of these additional prescribing barriers.
Nonetheless, SGLT2 inhibitor prescribing in our population at high cardiovascular risk was suboptimal. It often takes time for any new medication to achieve optimal uptake, as we found previously with statins.11,19 Moreover, there are multiple established cardioprotective medications for atherosclerotic CVD populations, along with hypertension, hyperlipidemia and diabetes management, which often take precedence. Adding an SGLT2 inhibitor may have been given a lower priority relative to traditional cardioprotective medications.7 In recognition of this barrier, calls to action have been issued to the cardiology community to provide education regarding and stimulate further adoption of SGLT2 inhibitors as cardioprotective agents.20
We found that the prescribing rate varied among different SGLT2 inhibitors, even though the cardioprotective efficacy has been considered as a class effect.4,7 This may have been owing to the timing of drug approval or publication of trial evidence (Appendix 1, Supplemental Table S4). Canagliflozin first received approval from Health Canada for management of type 2 diabetes, and it was the most frequently prescribed SGLT2 inhibitor in 2016/17. However, possibly owing to concerns about adverse effects (such as amputation) that were published in 2017, canagliflozin prescribing rates remained flat thereafter, whereas empagliflozin prescribing rates increased greatly, possibly because the cardioprotective evidence regarding this agent was published earliest among SGLT2 inhibitors.2 Our study showed early adoption of SGLT2 inhibitors, and further evaluation over a longer period will be needed, particularly since multiple randomized controlled trials have been published for various indications.5,6,21,22
We identified lower SGLT2 inhibitor prescribing rates in older people and those with concomitant CKD or heart failure, many of whom are at the highest risk for cardiovascular events.23 Although SGLT2 inhibitors are relatively well tolerated, it is possible that, in older patients with more comorbidities and polypharmacy, the risk of adverse effects such as genitourinary infections and risk of falls from hypotension could be higher.1–3 With close monitoring for potential adverse effects, the cardioprotective vascular benefit of SGLT2 inhibitors in atherosclerotic CVD and type 2 diabetes populations is still likely to outweigh potential risks in most older people. Furthermore, real-world evidence of the efficacy and safety of SGLT2 inhibitors in older populations (aged > 75 yr) is lacking, and further research in this population is warranted.
Prescribing of SGLT2 inhibitors among patients with an endocrinologist visit in the prior year was twice that among patients with a family physician visit and 10 times that among patients with a cardiologist visit. Given that SGLT2 inhibitors were developed as antihyperglycemics, endocrinologists are likely more familiar with prescribing SGLT2 inhibitors than other physicians. Furthermore, cardiologists may prioritize prescribing established and familiar cardioprotective agents. However, cardiologists are 4–5 times more likely to see patients with concomitant atherosclerotic CVD and diabetes than endocrinologists, which puts the former at the forefront of cardioprotective management for this population.24 Our findings highlight the need for cardiologists to heed the call to action by enhancing their SGLT2 inhibitor prescribing practices.
We found that markers of worse glycemic control in patients with diabetes were associated with greater likelihood of SGLT2 inhibitor prescribing. Since SGLT2 inhibitors are add-on antihyperglycemic agents, greater prescribing in those with worse diabetes control could be expected. However, given the clear evidence of cardioprotection, prescribing of SGLT2 inhibitors must move beyond add-on therapy for those with poor glycemic control, and these medications should be viewed as cardioprotective agents.
We identified sex and socioeconomic disparities in SGLT2 inhibitor prescribing. Men were 42% more likely than women to receive an SGLT2 inhibitor. In addition to the omnipresent sex disparities in prescribing of preventive cardiac medication, the risk of genital and urinary tract infections with SGLT2 inhibitors may further explain hesitancy to prescribe this agent to women.1,11,25 Finally, socioeconomic disparity was an independent risk factor for lower SGLT2 inhibitor prescribing, despite the nominal copay of $2/prescription for low-income older people in the health care system evaluated in this study. Underprescribing of evidence-based treatments in women and economically disadvantaged people was also more pronounced in our study than in prior SGLT2 inhibitor studies and those of other cardiac medications; this warrants further study.8,26
Limitations
With prescription claims data, we were unable to capture SGLT2 inhibitor prescriptions that were written but not filled by patients, which may have underestimated intended SGLT2 inhibitor prescribing. Our study cohort included patients with type 1 diabetes and those with type 2 diabetes. However, the proportion of type 1 diabetes in our diabetes database has been reported to be only 3.6%.15 Our data sets did not capture estimated glomerular filtration rate, and eligibility for SGLT2 inhibitor prescribing based on this parameter was not assessed. Furthermore, owing to the nature of administrative data, patient preference and rationale behind decisions were uncertain. Last, our data were restricted to people aged 65 years or older, and prescribing trends may differ in younger populations. However, our population-level data from a large cohort provide insights into overall patterns of SGLT2 inhibitor adoption in a population at high risk with concomitant diabetes and atherosclerotic CVD, for whom there is strong evidence that SGLT2 inhibitors improve cardiovascular outcomes.1–3
Conclusion
In a contemporary, real-world population of patients aged 65 years or older with diabetes and atherosclerotic CVD in a health care system without major cost barriers for patients, only 1 in 5 patients were prescribed an SGLT2 inhibitor, whereas statins were prescribed for 4 of every 5 patients. Although SGLT2 inhibitor prescribing increased over time, disparities in adoption by age, sex, socioeconomic status, comorbidities and physician specialty remained. Concerted efforts are needed to address potentially modifiable factors so that all eligible patients with type 2 diabetes and atherosclerotic CVD are able to realize the cardioprotective benefits of SGLT2 inhibitors. Specific strategies to enhance prescribing of these medications for women and for those with lower incomes, heart failure or CKD, and, in particular, by cardiologists are needed to optimize their use as cardioprotective agents to reduce cardiovascular morbidity and mortality.
Acknowledgement
The authors thank IVQIA Solutions Canada for use of their drug information file.
Footnotes
Competing interests: Jacob Udell reports grant support to his institution for clinical trial research from Boehringer Ingelheim and Janssen Pharmaceuticals, and honoraria for continuing medical education presentations from GlaxoSmithKline and Sanofi. He has participated on advisory boards for Boehringer Ingelheim, Sanofi and Novavax. No other competing interests were declared.
This article has been peer reviewed.
Contributors: All of the authors contributed to the study conception or design, data acquisition, analysis or interpretation. Aya Ozaki and Cynthia Jackevicius drafted the manuscript, and Dennis Ko, Alice Chong, Jiming Fang, Clare Atzema, Peter Austin, Therese Stukel, Karen Tu, Jacob Udell, David Naimark and Gillian Booth revised it critically for important intellectual content. All of the authors approved the final version to be published and agreed to be accountable for all aspects of the work.
Funding: Cynthia Jackevicius was funded by a Heart and Stroke Foundation of Canada Bridge Grant (G-20-0029363). Clare Atzema is supported by a Mid-Career Investigator Award from the Heart and Stroke Foundation, by Sunnybrook Research Institute and by the Department of Emergency Services, Sunnybrook Health Sciences Centre. Karen Tu received a Research Scholar Award from the Department of Family and Community Medicine, University of Toronto. Dennis Ko is supported by the Jack Tu Chair in Cardiovascular Outcomes Research, Sunnybrook Health Sciences Centre. Jacob Udell is supported by the Peter Munk Cardiac Centre, University Health Network; the Women’s College Research Institute and Department of Medicine, Women’s College Hospital; and the Department of Medicine, University of Toronto.
Data sharing: Although legal data-sharing agreements between ICES and data providers (e.g., health care organizations and government) prohibit ICES from making the data set publicly available, access may be granted to those who meet prespecified criteria for confidential access, available at https://www.ices.on.ca/DAS (email: das{at}ices.on.ca).
Disclaimer: This study was supported by ICES, which is funded by an annual grant from the Ontario Ministry of Health and Ministry of Long-Term Care. This document used data adapted from the Statistics Canada Postal CodeOM Conversion File, which is based on data licensed from Canada Post Corporation and/or data adapted from the Ontario Ministry of Health Postal Code Conversion File, which contains data copied under licence from Canada Post Corporation and Statistics Canada. Parts of this material are based on data and/or information compiled and provided by the Canadian Institute for Health Information and the Ontario Ministry of Health. The analyses, conclusions, opinions and statements expressed herein are solely those of the authors and do not reflect those of the funding or data sources; no endorsement is intended or should be inferred.
Supplemental information: For reviewer comments and the original submission of this manuscript, please see www.cmajopen.ca/content/11/3/E494/suppl/DC1.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/
References
- © 2023 CMA Impact Inc. or its licensors