Abstract
Background Outbreaks of SARS-CoV-2 in shelters and congregate living settings are a major concern because of overcrowding and because resident populations are often at high risk for infection. The objective of this study was to describe the development, implementation and assessment of the COVID-19 Community Response Team, a program that enabled Women’s College Hospital in Toronto, Ontario, to work in partnership with shelters and congregate living settings to prevent outbreaks.
Methods The Community Response Team, associated with Women’s College Hospital, an academic ambulatory hospital, carried out mobile testing for SARS-CoV-2, supported outbreak management and prevention through ongoing onsite partnership with medical staff, and conducted infection prevention and control (IPC) training to shelter staff. We conducted a descriptive analysis of the sites supported by the program between Apr. 20, 2020, and Aug. 15, 2020. We also assessed the program’s feasibility (number of completed needs assessments, mobile testing events and IPC training events, and median time from referral to service delivery), adoption (number of nasopharyngeal swabs, number of pre- and post-program outbreaks and IPC uptake) and acceptability or satisfaction.
Results The Community Response Team supported 32 sites. Of those, 30 completed an intake needs assessment, 24 completed mobile testing for SARS-CoV-2 and 15 received IPC support. Mobile testing resulted in the collection of 1566 nasopharyngeal swabs, of which 64 were positive for SARS-CoV-2 infection. Three sites had confirmed outbreaks. The median time from referral to needs assessment was 4 days (interquartile range [IQR] 1–13 days), and the median time to the testing day was 9 days (IQR 1–49 days). The median time from referral to IPC staff training was 14 days (IQR 4–79 days), and 100% of respondents reported being pleased or very pleased with the training. During the follow-up period, the 3 facilities with outbreaks overcame those outbreaks. Three sites supported by the Community Response Team had further single cases, but no site reported subsequent or secondary outbreaks.
Interpretation The Community Response Team program led to the transfer of IPC knowledge, allowed for the management and prevention of SARS-CoV-2 outbreaks, and demonstrated feasibility. Collaborative supports between hospitals and the community housing sector may serve as models for ongoing system integration beyond the COVID-19 pandemic.
Shelters in Toronto have been overcrowded for years, operating at an average nightly capacity of 98%; approximately 7000 people sleep in a shelter every night.1 Shelter residents have increased susceptibility to infection with SARS-CoV-2 because of crowded congregate living and sleeping arrangements, the sharing of personal objects, limited access to hygiene supplies and the closure of public washrooms.2,3 Furthermore, shelter residents often have concurrent mental health conditions, substance use disorders or underlying health conditions that put them at greater risk of poor adherence to public health directives and poor outcomes if they become infected with SARS-CoV-2.2,4
In April 2020, cases of COVID-19 surged among Toronto’s homeless, with at least 135 over 10 days, most of which came from a single refugee shelter.5 In response to this surge, Women’s College Hospital (WCH) launched the COVID-19 Community Response Team (CRT) on Apr. 20, 2020. This program partnered with shelters, congregate living settings and supporting organizations to manage and prevent outbreaks of SARS-CoV-2 using a comprehensive collaborative model instead of the “test and isolate” approach deployed in the general population. The CRT involved the following: helping to identify cases of SARS-CoV-2 infection through onsite mobile testing; supporting the management and prevention of outbreaks (2 weeks of ongoing follow-up with a medical lead from WCH who supported contract tracing, isolation, symptom management and subsequent testing needs); and providing infection prevention and control (IPC) training and guidance in shelters and congregate living settings.
In June 2021, Baral and colleagues6 published a systematic review of 22 articles that evaluated the implementation of programs aimed at preventing communicable diseases in shelters: 11 related to COVID-19, 3 to H1N1 influenza and 7 to tuberculosis. Similar to ours, these programs included testing (n = 12), screening (n = 9), IPC changes (n = 5) and isolation (n = 4), but only 2 included education.
Another meta-analysis of 37 studies (31 observational, 4 qualitative and 2 modelling) by Mohsenpour and colleagues7 showed a baseline SARS-CoV-2 prevalence of 2.32% in shelter residents and 1.55% in staff. During outbreaks, the pooled prevalence increased to 31.59% in residents and 14.80% in staff. The main IPC strategies described in these papers included universal rapid testing, expansion of non-congregate housing and in-shelter measures (bed spacing, limited staff rotation, reductions in the number of residents). However, none of these studies mentioned education or reported on the feasibility or effectiveness of the IPC strategies that were implemented.
The objectives of this article were to describe the development and implementation of the CRT and to assess its feasibility, its adoption and the related satisfaction of the community organizations, based on the first 32 sites involved in the program.
Methods
Design and setting
Located in Toronto, WCH is the only ambulatory academic hospital in Canada. In March 2020, the hospital set up one of Toronto’s 14 COVID-19 assessment centres to evaluate and test community members for SARS-CoV-2 infection. As an extension of the assessment centre, WCH partnered with Toronto shelters, congregate living settings and supporting organizations to develop and implement the CRT, a model of health care systems delivery to help manage and prevent COVID-19 outbreaks in those settings. The program was launched on Apr. 20, 2020, and it underwent cycles of adaptation to improve the model as the pandemic evolved. Organizations that received services from program inception to Aug. 15, 2020, were included in the present study.
We used descriptive analysis to assess feasibility, adoption and satisfaction. We also reported this study according to the Standards for Quality Improvement Reporting Excellence (SQUIRE) checklist, because the program was aimed at improving health care systems, access to care and community engagement.8
Program development
In April 2020, existing partnerships between WCH and Toronto shelters for refugees and the homeless prompted the expansion of the hospital’s Mobile COVID-19 Assessment Team (MCAT) — from testing in long-term care facilities to testing clients and staff in shelters and congregate living settings. The MCAT was deployed to these sites in collaboration with Toronto Public Health, and later with Ontario Health, the regional health authority.
Following the initial partnerships with shelters known to WCH, in June 2020 the hospital was assigned to the Toronto West area (geographical boundary assigned by Ontario Health) for future activities, including surveillance testing as directed by a newly formed Toronto Region COVID-19 roundtable. In anticipation of the need for expanded IPC training for new sites, WCH established the IPC Community Support Squad (CSS).
The MCAT handled onsite mobile testing and supported the management of outbreaks. The CSS liaised with sites to provide up-to-date, evolving COVID-19 resources, and it delivered IPC training and guidance to help prevent future outbreaks. The combined MCAT and CSS programs became the CRT.
To ensure that Indigenous Peoples were prioritized, the Centre for Wise Practices in Indigenous Health (CWP-IH), led by L.R. and S.M., joined the CRT. The CWP-IH is aimed at supporting the reclamation of Indigenous knowledge and governance. CWP-IH led and was involved in all CRT activities with Indigenous sites. The CWP-IH worked strategically to ensure that Indigenous referrals and requests were met in a timely and culturally safe manner. Historically tenuous relationships were tended and nurtured, and all CRT staff completed San’yas online Indigenous cultural safety training (www.sanyas.ca).
Program processes
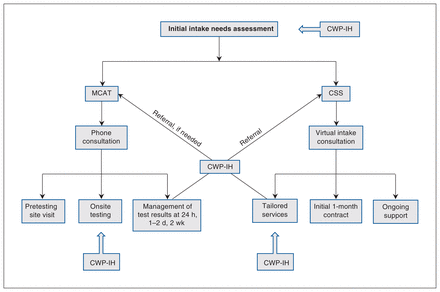
Figure 1 outlines the workflow of the CRT.
COVID-19 Community Response Team workflow. Workflow and its 3 components: the Centre for Wise Practices in Indigenous Health, the Mobile COVID-19 Assessment Team and the infection prevention and control Community Support Squad. The Community Response Team employed an evolving, iterative process through which sites were referred back and forth among the team’s 3 components based on need. Referrals were triaged centrally through a standardized intake needs assessment. Daily communication between Mobile COVID-19 Assessment Team and Community Support Squad project managers was essential to ensure effective workflow. Communication with Centre for Wise Practices in Indigenous Health leadership took place monthly. Note: CSS = Community Support Squad, CWP-IH = Centre for Wise Practices in Indigenous Health, MCAT = Mobile COVID-19 Assessment Team.
Referrals and needs assessments (CRT)
At first, referrals came from shelters that had outbreaks and had pre-existing partnerships with WCH (i.e., direct outreach from shelters to WCH leadership). However, referrals were quickly expanded to come from Toronto Public Health, Ontario Health or the CWP-IH. After shelter referral, a WCH senior executive (S.B.), the MCAT medical lead (S.L.), the MCAT program manager (L.B.) and the CSS program manager (V.L.K.) conducted an intake needs assessment.
The needs assessment tool captured site information such as capacity, target population, facility style (single room, dormitory, etc.), details on IPC and COVID-19 policies and procedures, the availability of personal protective equipment, and more (needs assessment tool available upon request). All information was transferred to a database in Excel (Microsoft). We used this needs assessment to determine whether the MCAT should first be deployed for urgent testing or whether the CSS should be deployed for IPC support. In June 2020, the MCAT also began surveillance testing in assigned Toronto West shelters under the direction of Ontario Health or Toronto Public Health.
Before services were provided, sites signed a letter of agreement developed by WCH.
Mobile testing (MCAT)
When a site was assigned to the MCAT, we employed a 5-step process: 1) an MCAT needs assessment before the testing day, and an in-person site visit to prepare for the testing day (which could be combined); 2) the testing day; 3) 24 hours after the testing day, when results were returned; 4) 1–2 days after the testing day for case management if any tests had positive results, and for isolation of cases and close contacts; and 5) a 2-week follow-up period of daily check-ins and screening for new symptoms that would warrant repeat testing.
IPC training and implementation support (CSS)
Sites that did not fulfill the requirements for MCAT deployment or that had already completed the MCAT process were offered CSS support. This process started with CSS intake using a standardized form (available on request) that collected details about the site, its IPC practices, and its needs. Based on this information, the CSS offered a package of support to each site tailored to its needs, including the following: virtual or in-person staff training on COVID-19 and IPC; virtual or in-person training on COVID-19 and IPC for clients or residents; sharing of IPC and case management tools and posters; and ongoing communication and support via email and phone.
The CSS training was based on IPC guidance published by Toronto Public Health, Public Health Ontario, and Ontario Health.9–11 Materials were distilled down to 6 IPC principles: screening (passive and active), hand hygiene, personal protective equipment, physical distancing, respiratory etiquette and cleaning and disinfecting (training material available upon request). To accommodate the influx of surveillance sites in June 2020, CSS developed a weekly webinar for community engagement and support in lieu of tailored support.
Program adaptations
Because of the rapid roll-out of the CRT, frequent adaptations were needed, including reducing the number of CRT members at the initial intake needs assessment, converting the MCAT intake process from 2 visits (1 by phone and 1 in person) to a single in-person visit, and reducing the tailored CSS offerings, when possible, from multiple tailored sessions to a single weekly webinar.
Participants
Sites that participated in this analysis included shelters that had previous relationships with WCH (n = 5) and shelters and congregate living sites in the Toronto West area as assigned to WCH. Community organizations that supported shelters and the homeless also participated and received CRT services (n = 2).
Data sources
We entered data from all needs assessments into a database in Excel. The MCAT recorded the number of nasopharyngeal swabs performed at each visit (residents and staff) and the positivity proportion; this information was reported to the program managers (V.L.K., L.B.) via email and entered into the Excel database. The CSS recorded the number of participants present at each training session; this information was reported to the program managers (V.L.K., L.B.) via email and entered into the Excel database.
Approximately 2 to 4 months after sites received service, a WCH staff member, trained in survey interview techniques, contacted site leads to administer a survey. (The team member was not part of MCAT testing or CSS training activities.) The survey included confirmation of recorded data, questions about satisfaction with CRT services and inquiries as to whether IPC practices had changed (Appendix 1, available at www.cmajopen.ca/content/10/2/E483/suppl/DC1). The survey was developed by M.L., M.K., G.M. and V.L.K. using a priori performance indicator questions12–14 and was reviewed and revised by team experts for content validity.15
Outcomes
This study was designed to assess feasibility outcomes, adoption and acceptability or satisfaction.16
Feasibility was defined as the extent to which an innovation is successfully used or carried out within a given agency or setting.17 Feasibility was determined by assessing the number of sites that received MCAT or CSS services and the median time from referral to service delivery.
Adoption was defined as the proportion of sites and staff that adopted our innovation of the CRT model.16,18 We assessed this using the number of nasopharyngeal swabs collected by the MCAT, the number of pre- and post-program outbreaks of COVID-19, the number of IPC training sessions conducted and resources provided, and the number of participants who attended. We also assessed adoption by asking how many IPC practices were adopted at each site after CSS training or interactions (i.e., the number of IPC practices added). We collected this information as part of the interviewer-administered survey described above.
As part of the survey, participants were asked about their satisfaction with the MCAT, CSS or both; if the team(s) met their needs; and if the site would recommend the MCAT or CSS to other organizations. Satisfaction was used as a measure of the acceptability of the innovation.
Statistical analysis
We conducted descriptive analyses using median and interquartile range (IQR) for continuous variables and frequency and proportion for categorical variables. Site names are not reported, and data are presented in aggregate form for confidentiality.
Ethics approval
We obtained approval from the WCH research ethics board chair through the Assessment Process for Quality Improvement Projects program (REB No. 2020-0068-E).
Results
From Apr. 20, 2020, to Aug. 15, 2020, the CRT engaged with 32 sites. Site characteristics are presented in aggregate in Table 1; individual site details (such as capacity) are presented in Appendix 1, Table S1. Of the 32 sites, 26 (81.3%) were shelters and most had a specialty focus. Eight sites (25%) served women, 4 sites (12.5%) served refugees and 3 sites (9.4%) were low-barrier sites (i.e., facilities that removed as many entry “exclusion criteria” as possible, aiming to support individuals often rejected by the shelter system).
Site characteristics*
Feasibility assessment
Of the 32 sites included in our analysis, 24 were first assigned to MCAT, 7 were first assigned to CSS and 1 was supported by both MCAT and CSS from the outset. The median time from CRT referral to the initial needs assessment was 4 days (IQR 1–13 days; n = 19 sites). The median time from the needs assessment to the MCAT testing day was 9 days (IQR 1–49 days; n = 25 sites). The median time from CRT referral to CSS intake was 4 days (IQR 1–33 days; n = 15 sites). The median time from CRT referral to CSS staff training was 14 days (IQR 4–79 days; n = 11 sites).
Adoption assessment
The MCAT conducted mobile testing at 28 sites. In total, 1566 nasopharyngeal swabs were collected (1189 in clients and 377 in staff); of those, 64 samples were positive for SARS-CoV-2 infection. As a result of testing, 3 sites were classified as having an outbreak (i.e., 2 or more positive cases19; Table 2). One site had a pre-existing outbreak that led to testing. Overall, the median number of swabs collected per testing day was 38 (range 7–153). The median number of swabs collected per day among clients was 33 (range 6–135), and the median number of swabs collected per day among staff was 11 (range 0–41). Except for 3 sites, the positivity proportion was low (Appendix 1, Table S1).
Adoption assessment
During the follow-up period, all sites overcame their outbreaks. Three had subsequent single positive cases, which led to repeat testing by the MCAT or another mobile testing team. One site underwent repeat testing by the MCAT because of a high positivity proportion at the initial testing.
The CSS carried out 15 in-depth intakes and supported all 15 sites with IPC training. Table 2 provides information about the services requested and which services were provided by the CSS. In total, the CSS conducted virtual staff training sessions for 11 sites, 4 in-person training sessions (including walk-throughs) and 1 virtual client education session, and they sent documents to 14 sites. Of the sites that responded to the survey, 100% had changed at least 2 IPC practices after the CSS training and 80% had changed more than 2.
Acceptability or satisfaction assessment
Table 3 summarizes the sites’ satisfaction with the CRT’s services.
Satisfaction assessment*
Of the sites that received services from the MCAT (n = 24), all (100%) were pleased or very pleased with those services. All (100%) agreed or strongly agreed that the MCAT met their needs, and all (100%) agreed or strongly agreed that they would recommend the services of the MCAT.
Of the sites that received services from the CSS (n = 15), all (100%) were pleased or very pleased with those services. All (100%) agreed or strongly agreed that the CSS met their needs, and all (100%) agreed or strongly agreed that they would recommend the services of the CSS.
Interpretation
The CRT is a hospital-led, community-partnering program created to help manage and prevent COVID-19 outbreaks in shelters, congregate living sites and supporting organizations. Analysis of the first 32 organizations that received services from the CRT showed that these sites found the program to be feasible and acceptable. Onsite mobile testing resulted in the collection of 1566 nasopharyngeal swabs, and of those, 64 were positive for SARS-CoV-2. Three shelters that experienced COVID-19 outbreaks were supported by the CRT, and no further outbreaks occurred between April 2020 and August 2020. The CRT provided comprehensive IPC training and support to 15 sites, leading to changes in more than 2 IPC practices among 80% of the sites. All sites reported satisfaction with and acceptability of the program, suggesting a great need for such services.
Other jurisdictions, such as South Korea, were quick to identify the need for mobile testing models.20 Mobile or onsite mass testing has been implemented successfully in workplaces and other types of congregate living facilities, such as treatment facilities and long-term care homes, with high uptake and efficacy in mitigating outbreaks.21–23 A Hamilton team rapidly developed partnerships between Mar. 19, 2020, and Apr. 30, 2020, and they collected a total of 245 nasopharyngeal swabs from 141 staff and 104 residents at shelters in the Hamilton region; they did not comment on IPC training.24 Similarly, the studies included in the systematic review by Mohsenpour and colleagues7 reported on SARS-CoV-2 testing and positivity proportions but did not describe any IPC training implemented.
The CRT learned that preparatory engagement activities (to create a testing model and establish support delivery that was responsive to each site) set the stage for the sites to engage optimally with the CRT. The CRT approach offered wraparound, ongoing IPC support that was adapted to the needs of each site. Other Toronto hospitals offered IPC training sessions to sites where mobile testing was being conducted, but these were limited to single sessions. Our finding that over 80% of teams changed more than 2 IPC practices after training suggests that the IPC support available to shelters had been limited beforehand, and that the training was an important program innovation. The tailoring of this support was furthered by the collaborative relationship between the CSS and the MCAT, through which colleagues were briefed on relationships and practices before a site was referred from one to the other.
As the COVID-19 pandemic continues, health care system innovations and adaptive models of care are needed to address the needs of shelters and congregate living settings. These sites will continue to face challenges in supporting clients who have various comorbidities and mental health needs, and who often resist COVID-19-related policies, such as mask-wearing. 2,25 With the influx of service users and the overall implications of reduced bed capacities, IPC and outbreak management needs are likely to continue for shelters. Given limited resources, the long-term gap is the sustainability of a program such as the CRT. Although a plan was initiated to transition the CRT to a partnering community health centre as of September 2020, the WCH continued to support shelters with testing needs up to December 2021.
Limitations
This study had several limitations. Owing to the rapid implementation of the CRT, several types of data were not captured. For example, referral dates and the number of participants at training sessions were not always recorded. The median intervals reported between referral and CRT needs assessment, and between referral and testing, may not fully reflect the nuanced way in which referrals were triaged when they were urgent, and the narrowing of this interval over time has not been reported. Additional nuances related to the interactions between the various CRT pillars and the detailed partnering relationships with community sites were not feasible in this study. Understanding these interactions would be valuable for establishing a similar program and for explicating why certain activities (such as testing and delivery of IPC support) were delayed. We did not assess cost in this study.
The present report does not include the perspectives of our Indigenous partners. Nonetheless, the integration of an Indigenous lens and Indigenous cultural safety training and considerations from the outset, led by CWP-IH, were essential for the success of the CRT. A strength of the CRT was exploration of community partnerships, which emerged through listening to sites’ needs, tailoring the program to those needs and meaningful relationship-building.
Conclusion
This study showed that a hospital-led, community-partnering comprehensive program to help manage and prevent COVID-19 outbreaks in shelters and congregate living settings was feasible and acceptable. Shelters are historically under-resourced and undervalued, but they are integral to the fabric of society in Canada. Without adequate support that is responsive to their unique needs, they are likely to continue to face important consequences from the COVID-19 pandemic. Collaborative programs between hospitals and the community housing sector should be explored as a health care systems innovation that could reduce outbreaks not only of COVID-19 but also of other respiratory viruses and future pandemics.
Acknowledgements
The authors would like to thank the staff and clients at all the shelters, congregate living settings, and supporting organizations for their collaboration and hard work, as well Toronto Public Health and the Inner-City Health Associates for working in partnership with them. They thank Public Health Ontario and the Ministry of Health, Ontario for their guidance documents. They would also like to thank Ms. Christal Malcolm, an administrative assistant in the Women’s College Hospital Department of Surgery, whose voluntary redeployment was instrumental in data collection.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
Contributors: Mona Loutfy, Logan Kennedy, Mina Kazemi, Sacha Bhatia and Danielle Martin contributed substantially to study conception and design. Mona Loutfy, Logan Kennedy, Sheila Riazi, Suvendrini Lena, Mina Kazemi, Jessica Bawden, Vanessa Wright, Lisa Richardson, Selena Mills, Laura Belsito, Geetha Mukerji, Meenakshi Gupta, Cristina Barrett and Danielle Martin contributed substantially to analysis and interpretation of the data. Mona Loutfy and Logan Kennedy wrote the article, and Sheila Riazi, Suvendrini Lena, Mina Kazemi, Jessica Bawden, Vanessa Wright, Lisa Richardson, Selena Mills, Laura Belsito, Geetha Mukerji, Sacha Bhatia, Meenakshi Gupta, Cristina Barrett and Danielle Martin revised the manuscript critically for important intellectual content. All authors approved the final version to be published and agree to act as guarantors for the work.
Data sharing: Data are available by emailing logan.kennedy{at}wchospital.ca.
Supplemental information: For reviewer comments and the original submission of this manuscript, please see www.cmajopen.ca/content/10/2/E483/suppl/DC1.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/
References
- © 2022 CMA Impact Inc. or its licensors