Abstract
Background: As the leading cause of emergency department visits in Canada, pain disproportionately affects socioeconomically disadvantaged populations. We examine the association between household food insecurity and individuals’ pain-driven emergency department visits.
Methods: We designed a cross-sectional study linking the Canadian Community Health Survey 2005–2017 to the National Ambulatory Care Reporting System 2003–2017. Food insecurity was measured using a validated questionnaire. We excluded individuals with missing food insecurity status, individuals younger than 12 years and jurisdiction-years with partial emergency department records. We assessed emergency department visits driven by pain at different sites (migraine, other headaches, chest–throat pain, abdomen–pelvis pain, dorsalgia, joint pain, limb pain, other pain) and their characteristics (frequency, cause, acuity and time of emergency department visit) in Ontario and Alberta. We adjusted for sociodemographic characteristics, lifestyle and prior non–pain-driven emergency department visits in the models.
Results: The sample contained 212 300 individuals aged 12 years and older. Compared with food-secure individuals, marginally, moderately and severely food-insecure people had 1.42 (95% confidence interval [CI] 1.20–1.68), 1.64 (95% CI 1.37–1.96) and 1.99 (95% CI 1.61–2.46) times higher adjusted incidence rates of pain-driven emergency department visits, respectively. The association was similar across sexes and significant among adults but not adolescents. Food insecurity was further associated with site-specific pain, with severely food-insecure individuals having significantly higher pain incidence than food-secure individuals. Severe food insecurity predicted more frequent, multicause, high-acuity and after-hours emergency department visits.
Interpretation: Household food insecurity status is significantly associated with pain-driven emergency department visits in the Canadian population. Policies targeting food insecurity may reduce pain and emergency department utilization.
Pain has grown more prevalent in high-income countries, including Canada and the United States, where 1 in 5 people report having chronic pain.1,2 Lack of pain clinics and long wait times have forced many to self-medicate — sometimes with illicit drugs — and to seek care at an emergency department.3 Abdominal and pelvic pain, pain in the throat and chest, and dorsalgia are among the most common causes of emergency department visits in Canada, jointly accounting for one-tenth of all visits.4 Pain may reduce quality of life and trigger or exacerbate substance abuse, anxiety and depression,5,6 precipitating suicide in extreme cases.7 Service delays and undertreatment at emergency departments are believed to contribute to risky self-medication by patients with pain.8 In the context of a health care system, poorly managed pain has been associated with increased health care utilization and costs.9
Food insecurity — inadequate or insecure access to food because of financial constraints — is a serious problem in Canada.10 The ongoing COVID-19 pandemic further aggravated the issue.11,12 As a well-established social determinant of health, food insecurity has been associated with multiple negative health outcomes, including mental disorders, substance use and suicide.13–18
Population research connecting food insecurity and pain is rare. As a notable exception, food insecurity has been associated with self-reported chronic pain among Canadian adults and adolescents in a graded fashion.19 Two other cross-sectional studies have associated food insecurity with self-reported migraine among Canadians and young adults in the US.20,21 A higher prevalence of pain has been documented among lower income and less educated populations,22–24 but those indicators do not necessarily capture food insecurity and its associated health hazards.
Food-insecure people may be more susceptible to pain than food-secure individuals because of their higher likelihood of having chronic diseases,14–17,25–28 stress29,30 and physically demanding jobs.22,31 Moreover, pain may be less manageable for food-insecure patients and more likely to require emergency department intervention because of cost-related nonadherence to pain-relieving prescriptions and therapy,32–34 suboptimal dietary intakes,35 hampered access to physicians owing to inflexible work schedules and residence location, 31,36–38 inadequate social support22,29 and discrimination.39 Two studies reported higher emergency department use among food-insecure adults in Ontario, Canada,16,40 and studies have found that food insecurity is associated with higher emergency department use in the US.41–43 None of these studies has examined the role of pain in emergency department visits.
Food-insecure people may use emergency departments more than their food-secure counterparts for reasons related to pain; however, evidence to date has either focused on self-reported pain or all-cause emergency department visits. 19–21,40–43 Understanding inequity in pain-driven emergency department use is necessary for effective pain management and sustainable health care. We linked a Canadian population survey to emergency department records to examine the association between the severity of household food insecurity and individual pain-driven emergency department visits.
Methods
Study design
We conducted a retrospective analysis of cross-sectional survey data linked to health administrative data. The study was reported according to the Reporting of Studies Conducted Using Observational Routinely-collected Data (RECORD).44
Data and sample
The Canadian Community Health Survey (CCHS) is an annual cross-sectional survey administered to roughly 65 000 households in Canada, with response rates of 60%–80%.45–47 One member aged 12 years or older is randomly selected per household to answer the survey. Indigenous people living on reserves, members of the Canadian Armed Forces, people living in institutions, children in foster care and people living in northern Quebec are excluded. The responses generalize to 98% of the noninstitutionalized population aged 12 years and older in the country. Questions on food insecurity have been formally incorporated in the survey since 2005, though certain provinces and territories chose not to include those questions when given the option.
The National Ambulatory Care Reporting System (NACRS) contains roughly 64% of administrative records on emergency department visits in Canada.48 The NACRS has collected records for all emergency department visits in Ontario since 2002, Alberta since April 2010, and Yukon since 2015. Records are partial for other jurisdiction-years. The NACRS provides case-level information on timing, type, severity, cause and disposition of each emergency department visit. Each visit is assigned 1 main cause — the problem deemed the clinically significant reason for the visit requiring evaluation or treatment or management — and up to 9 joint causes, all coded in the International Statistical Classification of Diseases and Related Health Problems, 10th Revision, Canada (ICD-10-CA).
We limited our sample to CCHS respondents interviewed from 2005 to 2017 in Ontario and those interviewed from April 2012 to 2017 in Alberta. The 2 provinces combined represent roughly half of the country’s population.49 This sampling strategy maximized sample size while enabling us to identify emergency department visits in the past 2 years for variable construction. Other jurisdiction-years were excluded because of potential sampling bias. For instance, the optional reporting of emergency department records to the NACRS by certain hospitals in Manitoba or pre-2010 Alberta may be related to lower neighbourhood income — a contextual predictor of food insecurity — compared with nonreporting hospitals in the same jurisdiction-years, leading to spurious associations between emergency department visits and food insecurity. We did not include Yukon because of its limited data on food insecurity.
We linked CCHS respondents to NACRS records from 2003 to 2017 through unique person identifiers; those without NACRS records were presumed to not have attended an emergency department during the observation period. The CCHS–NACRS linkage rates in the raw data are 89.73% for Ontario and 84.16% for Alberta.50 Of the survey respondents in Ontario and Alberta, we excluded those with invalid food insecurity data and those from Ontario during 2015–2016, given Ontario’s opt-out from food insecurity monitoring (Appendix 1, Supplementary eFigure 1, available at www.cmajopen.ca/content/10/1/E8/suppl/DC1).
Measurements
Our primary outcomes were number of emergency department visits because of any pain and pain at different sites (migraine, other headaches, chest–throat pain, abdomen–pelvis pain, dorsalgia, joint pain, limb pain and other miscellaneous pain), measured over the 12-month period before CCHS interviews (Appendix 1, Supplementary eTable 1). We used ICD-10-CA codes for the main cause of the visit to build count variables for pain to capture the frequency and incidence rate of pain-driven emergency department visits (Appendix 1, Supplementary eTable 2). Pain as a symptom of other illnesses was common but beyond our study’s scope; therefore, joint causes of the visit were disregarded in variable building.
We further constructed secondary outcomes on characteristics of pain-driven emergency department visits for the past-year patients. They included number of emergency department visits driven by pain, visits of high acuity (resuscitation, emergent or urgent, as opposed to semiurgent or nonurgent), visits with multiple causes (1 or more causes, with pain being the main cause) and visits after hours (weekdays 00:00–7:59 or weekends 16:00–7:59).
Our key exposure was past-year household food insecurity status, with the same 12-month reference period as the outcomes. This is a 4-level categorical variable built from the 18-item questionnaire in the CCHS, which was developed and validated by the United States Department of Agriculture and adapted by Health Canada.51 On the basis of the number of affirmative answers, a household is classified as either food secure or marginally, moderately or severely food insecure.51,52
We adjusted for factors that may confound the relation between food insecurity and pain-driven emergency department visits. These included respondents’ sex (male, female), age at interview (years), race or ethnicity (white, Black, Indigenous, others), immigrant status (Canadian-born, immigrant), tobacco smoking status (never, former, current), past-year alcohol consumption (none, up to once a week, more than once a week) and number of emergency department visits not driven by pain in the year before (13–24 months ago). We also controlled for household characteristics, such as highest education (high school incomplete, high school diploma, some college, college degree), housing tenure (renter, homeowner), household type (couple with children, couple without children, lone parent, other), province (Ontario, Alberta) and survey cycle. These variables have been found predictive of pain or emergency department use.16,20,21,23,24,40–43 Missing values for covariates were rare (< 1% except education [4.4%]); therefore, for simplicity, we coded them as separate categories within each variable.53
Statistical analysis
We first described sample characteristics by emergency department visit status and computed crude incidence rates of emergency department visits because of any pain and site-specific pain across food insecurity levels. To ascertain the significance of between-group differences, we applied Student t tests for continuous variables and χ2 tests for categorical variables.
Owing to overdispersion (Pearson goodness-of-fit χ2 p < 0.001), we fitted negative binomial models on the count outcomes adjusting for confounding factors. Pain and emergency department use vary across demographic groups;4,23,24 thus, we also stratified our analyses on overall pain-driven emergency department visits by sex and age. We computed average predicted probability of the primary outcomes based on the adjusted models using marginal standardization. We then fitted adjusted negative binomial models on the secondary outcomes for the pain-driven emergency department visits.
We conducted sensitivity analyses expanding the sample to incorporate partial records from all jurisdictions, testing Poisson and zero-inflated negative binomial models, adjusting for household income, and experimenting with a broader definition of pain, considering diseases commonly associated with chronic pain, such as fibromyalgia.
We computed 2-sided confidence intervals (CIs) and set the significance at p < 0.05. All analyses were done with the sampling weights of CCHS in Stata SE 15.1. Numbers of observations were rounded to protect identity. Data and programming codes are stored in Statistics Canada’s Research Data Centre with restricted access.
Ethics approval
We obtained ethics approval from the Health Sciences Research Ethics Board at the University of Toronto.
Results
After excluding 29 200 individuals with missing data on food insecurity, we reached the final sample of 212 300 individuals aged 12 years and older in Ontario and Alberta (Appendix 1, Supplementary eFigure 1). Of these, 12 000 had 1 or more pain-driven emergency department visit in the year before interview. After application of survey weights to obtain population estimates, of the 212 300 sampled respondents, 7600 (3.9% of represented population), 10 400 (5.5%) and 5400 (2.5%) lived in marginally, moderately and severely food-insecure households, respectively (Table 1). A total of 115 600 (50.8%) women were in the sample. The average age at interview was 43.8 (standard deviation 19.0) years. Patients seen in the emergency department were socioeconomically more disadvantaged than nonvisitors (e.g., lower income, less education).
Sample characteristics by past-year pain-driven emergency department visit status among respondents of the Canadian Community Health Survey 2005–2017
The incidence rate of pain-driven emergency department visits was 62 per 1000 person-years (Table 2). The comparable figures were 55 for food-secure individuals and 85, 109 and 167 for marginally, moderately and severely food-insecure individuals, respectively. Pain-driven emergency department visits were more common among women than men (p < 0.05 for all but moderately food-insecure people) and more common among adults than adolescents younger than 18 years (p < 0.05 for all). Abdomen–pelvis pain, chest–throat pain and dorsalgia were the most common types of pain driving emergency department visits.
Incidence rate per 1000 person-years of past-year all-cause and pain-driven emergency department visits in the overall sample and of characteristics of pain-driven visits among past-year pain-driven emergency department visitors, by food insecurity status*
Among those patients seen in the emergency department, each had on average 1.33 pain-driven emergency department visits, 0.39 visit with multiple causes, 0.90 high-acuity visit and 0.82 visit during after-hours. Pain-driven emergency department visits were more common among those experiencing more severe food insecurity regardless of pain type, sex or age, with all trends significant at p < 0.05 except for adolescents 12–17 years old (p = 0.3). Patients seen for pain were also more likely to make more frequent, multicause, high-acuity and after-hours emergency department visits if they were food insecure versus food secure (trends p < 0.05).
Regression results
Marginal, moderate and severe food insecurity were associated with 1.55 (95% CI 1.32–1.84), 1.99 (95% CI 1.62–2.44) and 3.05 (95% CI 2.50–3.71) times higher incidence rates of pain-driven emergency department visits, respectively (Table 3). The rate ratios shrank to 1.42 (95% CI 1.20–1.68), 1.64 (95% CI 1.37–1.96) and 1.99 (95% CI 1.61–2.46), respectively, after adjustment for confounders (Appendix 1, Supplementary eTables 3 and 4). The association was significant for males and females, and for adults younger than 65 years and adults aged 65 years and older (except for moderate food insecurity). No association with food insecurity was significant among adolescents.
Negative binomial models on past-year pain-driven emergency department visits in the overall sample and by sex and age subsamples*
Broadening the definition of pain, adding partial emergency department records from other jurisdictions, adjusting for income, or fitting a Poisson or zero-inflated negative binomial model barely changed the results (Appendix 1, Supplementary eTable 5).
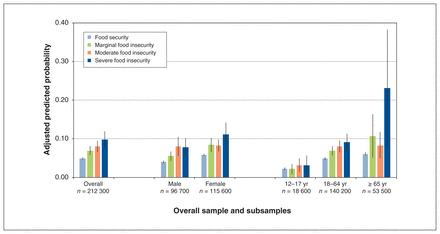
With few exceptions, females and adults tended to have higher incidence rates of pain-driven emergency department visits than their male and adolescent counterparts, respectively (Figure 1). However, neither sex nor age significantly moderated the association between food insecurity and pain-driven emergency department visits after confounders adjustment (all interactions p > 0.05).
Adjusted predicted probability of past-year pain-driven emergency department visits by food insecurity status, in overall sample and by sex and age subsamples. All models adjusted for sex, age, race or ethnicity, immigrant status, highest education in household, housing tenure, household type, jurisdiction of residence, smoking status, past-year alcohol consumption, Canadian Community Health Survey cycle and frequency of non–pain-driven emergency department visit in the year before. Black vertical lines indicate 95% confidence intervals.
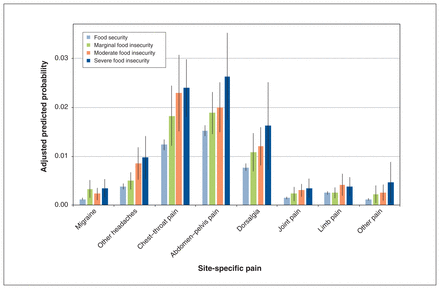
A graded association between food insecurity status and site-specific pain was found in the unadjusted models, with a more severe level of food insecurity linked to a greater incidence rate of emergency department visits because of pain at different sites (Table 4; Appendix 1, Supplemental eTable 6). After adjustment for confounding factors, the graded association with food insecurity status by and large persisted. Moderate and severe food insecurity were associated with pain at all sites except limb pain. Marginal food insecurity was significantly associated with migraine and chest–throat pain only. Abdomen–pelvis pain and chest–throat pain were the most likely causes behind pain-driven emergency department visits for food-secure and food-insecure people alike after confounders adjustment (Figure 2).
Unadjusted and adjusted negative binomial models on past-year emergency department visits because of site-specific pain in overall sample (n = 212 300)*
Adjusted predicted probability of past-year emergency department visits driven by site-specific pain, by food insecurity status in overall sample (n = 212 300). All models adjusted for sex, age, race or ethnicity, immigrant status, highest education in household, housing tenure, household type, jurisdiction of residence, smoking status, past-year alcohol consumption, Canadian Community Health Survey cycle and frequency of non–pain-driven emergency department visit in the year before. Black vertical lines indicate 95% confidence intervals.
Among patients with a pain-driven emergency department visit in the past year (n = 12 000), moderate food insecurity was associated with more frequent (adjusted rate ratio 1.13, 95% CI 1.01–1.25) and after-hours (adjusted rate ratio 1.20, 95% CI 1.04–1.40) pain-driven emergency department visits. Severe food insecurity was associated with more frequent (adjusted rate ratio 1.32, 95% CI 1.15–1.50), multicause (adjusted rate ratio 1.50, 95% CI 1.19–1.88), high-acuity (adjusted rate ratio 1.37, 95% CI 1.17–1.61) and after-hours (adjusted rate ratio 1.29, 95% CI 1.10–1.51) pain-driven emergency department visits (Table 5; Appendix 1, Supplemental eTable 7). Marginal food insecurity was not significantly related to characteristics of emergency department visits.
Adjusted negative binomial models on characteristics of emergency department visits among pain-driven visitors*
Interpretation
Using multiyear emergency department records from 2 populous Canadian provinces, we found that food insecurity status was associated with pain-driven emergency department visits in a graded fashion. The association was similar across sex and age, and significant among adults but not adolescents. Among patients with pain-driven emergency department visits, severe food insecurity was associated with more frequent, multicause, high-acuity and after-hours visits.
The results are consistent with past literature on pain and emergency department visits, further confirming food insecurity as a determinant of health and health service use.14–21,40–43 The alignment of our findings with the literature highlights the disproportionate burden that food insecurity places on the Canadian health care system.15,16 Although pain is more prevalent among women than men for biological and social reasons,23 food insecurity affected both sexes’ risk of pain-driven emergency department visits similarly. Adolescents’ use of emergency departments for pain is rare compared with adults’ use and, as shown in population research in Canada and elsewhere, often related to sports or recreational injury rather than economic disadvantages,23,54 which may explain the null association of food insecurity with pain-driven emergency department visits among adolescents. An earlier study found that adults visiting the emergency department for chest pain were more than twice as likely to die in 5 years as those of similar ages without chest pain, mostly because of ischemic heart disease.55 Whether food insecurity aggravates the association between pain and more serious clinical outcomes, such as death, warrants investigation.
The association of food insecurity with headaches aligns with past findings20,21 and reinforces the notion that chronic stress and mental health problems are among the most salient health challenges facing food-insecure people.15–17 Both migraine and tension headaches have been prospectively associated with depression and other mental disorders.56 Chronic stress, common among food-insecure families, is a key determinant of the migraine–depression comorbidity.57 Headaches may mediate the association between food insecurity and mental health problems, yet more research is needed to assess this possibility.
Body pain often signals undiagnosed morbidities.58 Cancer, nervous system injury (e.g., stroke), and damage to or inflammation of organs (e.g., ischemic heart disease) can all cause severe pain, especially at later stages,58 when socioeconomically disadvantaged individuals are more likely to receive diagnoses of cancer and other chronic diseases than their less disadvantaged counterparts.59 Pain-driven emergency department visits may be the first opportunity to detect pain-related chronic diseases for a disproportionate share of food-insecure patients, which is a hypothesis awaiting validation. The correlations between severe food insecurity and joint and back pain may be related to overexertion caused by strenuous low-wage work.22,31
Food-insecure patients had more after-hours emergency department visits than their food-secure counterparts, which may relate to their greater probability of having inflexible work schedules (e.g., no sick leave) and less manageable pain (e.g., unable to wait until daytime hours). The reduced emergency department staff after hours may subject food-insecure patients to less effective pain management than they would have obtained during daytime hours, a hypothesis awaiting validation. Repeated, high-acuity and multicause emergency department visits for pain may indicate that complications of chronic conditions become more likely as food insecurity worsens to the severe level.15,60
Our study connected food insecurity to pain-driven emergency department visits, with plausible research and policy implications. The evidence so far suggests that food insecurity may magnify health problems, warranting policy interventions. Income supplements to low-resource populations have been effective in lowering food insecurity.61–65 Further investigation is needed to evaluate the effects of income supplements on pain and emergency department use.
Frequent visits to the emergency department may indicate inadequate access to other health care services, such as primary care. Researchers and policy-makers need to assess food-insecure patients’ access to primary care, as it may help reduce the burden on the emergency department. Virtual visits have shown promising signs of replacing, at least partly, in-person primary care;66 meanwhile, increasing after-hours physician services has moderately lowered use of emergency departments.67 These discussions are especially meaningful during the ongoing pandemic when food insecurity is rising while in-person meeting is minimized. However, accessibility of technology for virtual consultation (e.g., broadband Internet) remains questionable for socioeconomically disadvantaged populations.68
Moreover, it is important to lower the financial barriers to prescription pain relievers and pain management services, such as physiotherapy and psychotherapy. Physicians in Canada have raised concerns about dispensing of opioid-based analgesics in light of the rampant opioid crisis disproportionately hurting marginalized groups,69 especially food-insecure people.19 However, out-of-pocket expenses on non-opioid treatment may hinder proper pain management at early stages32,70 and increase the burden on the health care system by forcing patients with pain into free-of-charge, yet resource-intensive, emergency department use and hazardous coping strategies, such as illicit opioid use.71
Limitations
Our findings need to be interpreted with caveats. The results are correlational; the cross-sectional design prevents us from establishing causal directions. The possibility of unobserved confounders having led to food insecurity and emergency department visits simultaneously cannot be ruled out. Other data sets may allow examination of potential mediating effects of occupation, injury and chronic diseases on the correlation between food insecurity and pain-driven emergency department visits. Adjusting for prior emergency department visits could not eliminate selection bias; longitudinal data with repeated measurements of food insecurity are needed to ascertain causality. Moreover, although adding in partial records from all jurisdictions did not affect the results, our sample was in essence restricted to the individuals with measurement of food insecurity in Ontario and Alberta. Future studies may validate our findings elsewhere.
Conclusion
Household food insecurity status is significantly associated with pain-driven emergency department visits in the Canadian population. Policies targeting food insecurity may reduce pain and health care utilization, warranting further research.
Acknowledgements
This research was conducted at Toronto Research Data Centre, a part of the Canadian Research Data Centre Network. This service is provided through the support of the University of Toronto, the Canada Foundation for Innovation, the Canadian Institutes of Health Research, the Social Sciences and Humanities Research Council, and Statistics Canada. All views expressed in this work are the authors’ own. The authors thank the Canadian Institutes of Health Research for funding. The authors thank the reviewers for their constructive feedback.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
Contributors: Fei Men, Valerie Tarasuk and Marcelo Urquia contributed to the conception of the study. Valerie Tarasuk acquired the data. Fei Men designed the study, analyzed and interpreted the data, prepared the tables and figures, and drafted the manuscript. Valerie Tarasuk, Marcelo Urquia, and Fei Men revised the manuscript for important intellectual content. All authors gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Funding: This study was supported by the Canadian Institutes of Health Research grant PJT 153260, awarded to Valerie Tarasuk and Marcelo Urquia. The funder had no role in the design and conduct of the study; collection, management, analysis and interpretation of data; or preparation, review, decision to submit for publication or approval of the manuscript.
Data sharing: Data from this study cannot be shared publicly owing to the confidentiality agreement between Statistics Canada and respondents of the Canadian Community Health Survey. Data are available from the Statistics Canada Research Data Centre (telephone 905-525-9140 ext. 23661) for researchers who meet the criteria for access to confidential data.
Supplemental information: For reviewer comments and the original submission of this manuscript, please see www.cmajopen.ca/content/10/1/E8/suppl/DC1.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/
References
- © 2022 CMA Impact Inc. or its licensors