Abstract
Background: The COVID-19 pandemic was associated with increased mental health problems in the general population, yet psychiatric hospital admissions decreased. Early evidence suggested that psychiatric admissions normalized within weeks; we sought to examine the longer-lasting impacts on the psychiatric inpatient population beyond this initial period.
Methods: We compared Ontario Mental Health Reporting System admission data for patients admitted to 8 psychiatric hospitals in Ontario, Canada, between 3 time periods — before restrictions were imposed (June 22, 2019, to Mar. 16, 2020), during restrictions (Mar. 17 to June 21, 2020) and after restrictions were lifted (June 22, 2020, to Mar. 16, 2021) for changes in involuntary status, diagnoses and clinical presentation using descriptive analysis. For clinical presentation, we extracted scores on 4 Resident Assessment Instrument–Mental Health symptom scales (Depressive Severity Index, Cognitive Performance Scale, Positive Symptoms Scale–Long Version and Social Withdrawal Scale), and 2 behaviour scales (Aggressive Behavior Scale and Violence Sum).
Results: A cross-sectional sample of 9848 patients was included in the analysis. The mean number of daily admissions decreased 19% from 16.4 (standard deviation [SD] 8.0) before the restriction period to 13.3 (SD 6.1) during the restriction period, and was still 6% below prerestriction levels after restrictions were lifted 15.4 (SD 6.8), with standard error difference of 1.03 (95% confidence interval −0.22 to 2.29). From the pre- to the postrestriction periods, the proportion of involuntary patients increased by 6 percentage points, and the proportions of patients diagnosed with a psychotic disorder or personality disorder increased by 4 percentage points and 1 percentage point, respectively.
Interpretation: Psychiatric admissions did not fully return to prerestriction levels in absolute rates and patient acuity after COVID-19 restrictions were lifted. Psychiatric services must prepare to appraise and respond to any increased acuity through interventions for patients, workforce planning and mental health support for staff.
The World Health Organization declared COVID-19 a pandemic on Mar. 11, 2020.1 Despite increases in anxiety and depression in the general population during the pandemic,2–4 psychiatric services were often limited to urgent care, resulting in fewer admissions during the initial period of restrictions.5–8 Within 12 weeks, admission rates approached prerestriction levels;9–11 however, there is little research into whether this apparent recovery continued in the long term. Furthermore, increased rates of psychosis and mania12–14 and suicidal behaviour9,10 suggest increased acuity of the admission population, which is important information for planning clinical services (e.g., staffing ratios, skill sets, interventions). Evidence of increased involuntary admissions6,15–17 also suggests an added burden to hospitals given their association with acute illness and aggression,18,19 longer stays, readmissions20 and use of restraints.21
In Ontario, Canada, rates of admission to psychiatric hospitals for psychotic and substance-related disorders approximated prerestriction levels by the time initial COVID-19 restrictions were eased, in June 2020.11 In contrast, admissions for mood-, trauma- and stressor-related disorders had not yet returned to normal.11 Involuntary admissions were increasing before COVID-19,18 but whether this trend has continued is unclear. Thus, there is a need to examine whether changes in admission patterns and characteristics were sustained in order to effectively plan for inpatient psychiatric services under the now-prolonged pandemic timeline. The few existing longer-term studies did not distinguish between the initial restriction and postrestriction periods,13,16 did not investigate involuntary admissions11 or ended in mid-2020.9,10
In the current study, we aimed to examine changes in psychiatric admissions and the legal status of patients admitted to psychiatric hospitals in Ontario from the prerestriction period to the postrestriction period, up to March 2021. We included measures of inpatient acuity and burden (i.e., clinical presentation). We hypothesized that the admission rate would have decreased during the restriction period but have approximated the prerestriction rate in the postrestriction period; that the involuntary admission rate would have increased during the restriction period but have approximated the prerestriction rate in the postrestriction period; and that measures of clinical presentation would show higher acuity during the restriction period than during the prerestriction period but have approximated prerestriction levels after restrictions were lifted.
Methods
Setting
During the global health emergency, fear of COVID-19 exposure in hospitals deterred patients from seeking health care, which caused substantial disruption in the health care system, including a decreased volume of psychiatric admissions and acute psychiatric care. The Ontario government declared a state of emergency and imposed province-wide restrictions on Mar. 17, 2020, that closed nonessential businesses, indoor recreational programs, schools, public libraries, theatres and outdoor recreational spaces (e.g., parks, trails), and restricted travel and gatherings.22 We examined the impact of these conditions on psychiatric health care services by comparing inpatient admissions and acuity before restrictions were imposed, during the restriction period and after restrictions were lifted. We defined the restriction period to have begun when Ontario’s state of emergency was declared, reflecting the most stringent constraints, and the postrestriction period as of the date of Ontario’s stage 2 reopening (June 22, 2020), when most indoor services and outdoor spaces reopened except in a small, localized area. We accessed a cross-section of civil psychiatric patient admissions encompassing 8 Ontario psychiatric hospitals that provide acute and longer-term adult mental health services in Ontario’s 6 health regions — North East, North West, East, Central, West and Toronto region — including the 4 largest specialty psychiatric hospitals, which encompass two-thirds of Ontario’s psychiatric beds.
We first viewed weekly admission rates for Jan. 1, 2019, through Dec. 31, 2021 to examine admission rate changes in the context of seasonal variation. To compare equal pre- and postrestriction durations and calendar months within our available data, we then analyzed admission and patient data between the restriction period (Mar. 17 to June 21, 2020 [97 d]), the postrestriction period (June 22, 2020, to Mar. 16, 2021 [268 d]) and the prerestriction period (June 22, 2019, to Mar. 16, 2020 [269 d]).
Variables
We used data extracted from the Ontario Mental Health Reporting System, which incorporates the Resident Assessment Instrument–Mental Health (RAI–MH),23 and demographic and clinical data on all adult admissions to psychiatric inpatient hospitals in Ontario. The RAI–MH is a standardized clinical instrument used to regularly assess psychiatric inpatients. It has adequate interrater reliability (average percent agreement across all items > 80%)24 and convergent validity reported for clinical scales.25
We coded inpatient status at admission as voluntary or involuntary. Involuntary admissions included applications or orders for a psychiatric assessment (Form 1 or Form 2), involuntary (Form 3 or Form 4), and informal status (admitted with designated decision-maker consent).
We collapsed primary psychiatric disorders in the fifth edition of the Diagnostic and Statistical Manual of Mental Disorders26 into 7 categories: schizophrenia and other psychotic disorder, substance use disorder, mood or anxiety disorder, neurocognitive disorder, personality disorder, neurodevelopmental disorder and other disorder.
For clinical presentation, we extracted scores on 4 RAI– MH symptom scales and 2 behaviour scales, as documented by staff from observations during the first 3 days of admission. The Depressive Severity Index has 5 items (e.g., negative statements, expressions of guilt/shame), each scored from 0 (not present) to 3 (present daily), for a total score of 0–15. Depression severity scores of 3 or higher double the likelihood of a mood disorder diagnosis and is considered clinically meaningful.24 The Cognitive Performance Scale consists of 4 items concerning short-term memory/recall, daily decision-making, making oneself understood and self-performance in eating; scores range from 0 (intact) to 6 (very severe impairment), and a score of 3 or higher increases the likelihood of a dementia diagnosis by 14 times.24 The Positive Symptoms Scale–Long Version contains 8 items (e.g., hallucinations, inflated self-worth), each scored from 0 (not present) to 3 (present daily), for a total score of 0–24.27 The Social Withdrawal Scale has 6 items (e.g., decreased energy, reduced interaction), each scored from 0 (not present) to 3 (present daily), for a total score of 0–18.27,28 Finally, the Aggressive Behavior Scale includes 4 items (e.g., verbal abuse, physical abuse), each scored from 0 (not exhibited) to 3 (exhibited daily), for a total score of 0–12,27,29 and Violence Sum sums 3 items (violent acts, intimidation, ideation), scored from 0 (never) to 5 (in the previous 3 d), for a total score of 0–15 (unpublished data, 2016). Research in multiple settings and locations has shown that RAI–MH scales meet internal consistencies (α ≥ 0.7025), with average interrater agreement (κ = 0.7030).
Our primary outcomes of interest were differences between the prerestriction and postrestriction periods in daily admission rates, proportion of involuntary and voluntary admissions, and 7 categories of psychiatric diagnosis. Our secondary outcomes were the differences between the 2 periods in the 6 clinical scale scores.
Statistical analysis
We first charted weekly admission rates for Jan. 1, 2019, through to Dec. 31, 2021. We then generated descriptive statistics for the equal prerestriction and postrestriction periods, as well as the restriction period, for daily admission rates, sociodemographic variables, diagnoses, inpatient status, clinical presentation and length of stay, including mean and standard deviation (SD) for age and number of daily admissions, median and interquartile range (IQR) for length of stay, and number and proportion for categoric variables. To examine the significance of changes in admission rates, we calculated standard errors of the difference between the 3 periods (prerestriction, restriction and postrestriction). We used one-way analysis of variance with post hoc comparisons using Bonferroni corrections to test for differences in clinical scale scores across time periods and χ2 tests with Bonferroni adjustment with a critical p value of 0.00625 for categoric measures (i.e., diagnosis, involuntary status) to determine the significance for multiple comparisons. We converted scale scores to Z-scores to allow for easier interpretation of each scale and comparison of scale scores between periods.
Ethics approval
This study is part of a project investigating changes in the prevalence and correlates of mental health disorders in psychiatric inpatients using the RAI–MH that received approval from the authors’ institutional research ethics board with a waiver of patient consent based on the Tri-Council Policy Guidelines for waiver of consent (HPRA 19.12.03). Informed consent was not obtained given our retrospective, secondary analysis of anonymized data.31
Results
This was a complete data set with no missing data. We identified 11 593 admissions, of which 310 (2.7%) were excluded owing to no unique identification and 1435 were repeat admissions (accounting for 6.1%, 0.9% and 6.0% of the prerestriction, restriction and postrestriction admissions, respectively). The final sample thus consisted of 9848 cases. There were 5423 male patients (55.1%), 4411 female patients (44.8%) and 14 nonbinary patients (0.1%). The majority of patients (6695 [68.0%]) had never been married. The mean age was 42.7 (SD 18.2) years, and the median length of stay was 19 (IQR 9–50) days.
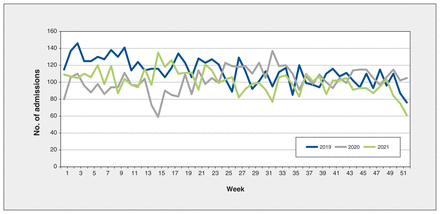
Of the 9848 patients, 4425 were admitted in the prerestriction period, 1291 during the restriction period and 4132 in the postrestriction period. The mean number of daily admissions decreased by 19% between the prerestriction and restriction periods (16.4 [SD 8.0] v. 13.3 [SD 6.1]), and by 6% between the prerestriction and postrestriction periods (16.4 [SD 6.8] v. 15.4 [SD 6.1]). The standard error difference between the prerestriction and restriction periods was 3.14 (95% confidence interval [CI] 1.58 to 4.70), between the pre- and postrestriction periods 1.03 (95% CI −0.22 to 2.29), and between the restriction and postrestriction periods −2.11 (95% CI −3.57 to −0.65), confirming our hypothesis that the admission rate would have decreased during the restriction period but approximated the prerestriction rate after restrictions were lifted. Figure 1 depicts weekly admissions between Jan. 1, 2019, and Dec. 31, 2021.
Number of weekly civil psychiatric admissions to 8 psychiatric hospitals in Ontario in 2019, 2020 and 2021. Weeks displayed are 7-day intervals in a calendar year with the exception of week 52 (includes 8 d in 2019 and 2021, and 9 d in 2020). Note: for figures depicting admissions for weeks 1–14, 15–25 and 26–52, see Appendix 1, Figures S1–S3 (available at www.cmajopen.ca/content/11/5/E988/suppl/DC1).
Legal status and diagnosis
The proportion of involuntary admissions increased significantly between the prerestriction and restriction periods (p < 0.001), and this trend was sustained in the postrestriction period. The proportion of involuntary admissions increased by 6 percentage points between the pre- and postrestriction periods (2164/4425 [48.9%] v. 2277/4132 [55.1%]) (Table 1), partially consistent with our hypothesis that the involuntary admission rate would have increased during the restriction period but approximated the prerestriction rate in the postrestriction period. Correspondingly, the proportion of patients admitted voluntarily decreased by 6 percentage points between the 2 periods (2261/4425 [51.1%] v. 1855/4132 [44.9%]).
Changes in admission status and diagnoses during the COVID-19 restriction and postrestriction periods*
The proportion of patients diagnosed with psychotic disorder increased significantly between the prerestriction and restriction periods (p < 0.001) and remained increased in the postrestriction period compared to the prerestriction period, by 4 percentage points (Table 1). Although admissions for patients with personality disorder were relatively infrequent, they also increased significantly between the prerestriction and and postrestriction periods (p < 0.001). There was a corresponding reduction in the restriction period in the proportions of patients with mood/anxiety disorder, substance use disorder and neurocognitive disorder, which was sustained in the postrestriction period for substance use disorder and neurocognitive disorder only.
Clinical presentation
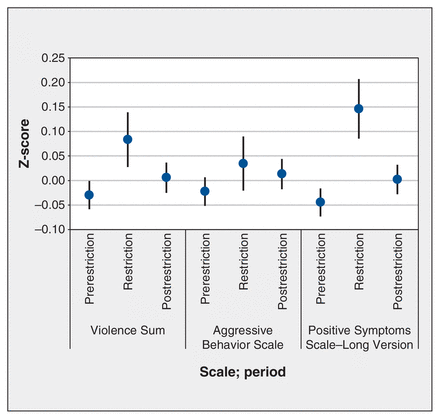
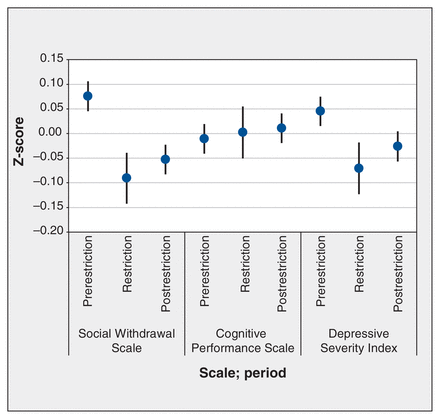
Mean scores only for depression and social withdrawal symptoms were significantly reduced during the restriction period and did not return to prerestriction levels in the postrestriction period (Table 2, Figure 2), partially consistent with our hypothesis that measures of clinical presentation would show higher acuity during the restriction period than during the prerestriction period but would have approximated prerestriction levels after restrictions were lifted. Patients exhibited more positive symptoms and violence during the restriction period than during the prerestriction period; however, these values were no longer significantly elevated in the postrestriction period, again consistent with our hypothesis. There was no difference in patients’ cognitive performance ratings and aggression scores across time (Table 2, Figure 3).
Changes in clinical presentation during the COVID-19 restriction and postrestriction periods*
Z-scores for clinical presentation measures of violence, aggression and positive symptoms per time period. Error bars represent 95% confidence intervals. Note: for figures depicting mean Z-scores for each clinical scale, March through June, see Appendix 1, Figures S4–S6.
Z-scores for clinical presentation measures of social withdrawal, cognitive performance and depression per time period. Error bars represent 95% confidence intervals. Note: for figures depicting mean Z-scores for each clinical scale, March through June, see Appendix 1, Figures S7–S9.
Interpretation
We found that the previously reported decrease in daily psychiatric hospital admission rates during COVID-19 restrictions10,13,14 were partly sustained in the remaining year after restrictions were lifted. Although total admissions for all diagnostic groups decreased during the restriction period, evidence that the proportion of patients with psychotic disorders and involuntary admissions increased substantially, and that patients scored higher on measures of positive symptoms and violence, indicates an increased burden on psychiatric services. The sustained predominance of psychotic disorder diagnoses and involuntary admissions after restrictions were lifted suggests an ongoing elevated operational burden on psychiatric hospitals. Mean scores on measures of depression and social withdrawal decreased during the restriction period and subsequently did not return to prerestriction levels; nevertheless, average scores remained at a clinically concerning level.
An increase in involuntary admissions is concerning because these admissions create an administrative burden, are distressing to patients’ informal caregivers32 and may represent a failure of psychiatric treatment.33 Increases in diagnoses and symptoms of psychosis suggest that the inpatient population is more mentally ill and requires more intensive treatment.34 Thus, psychiatric admissions may have returned to prepandemic rates, but each admission may now be more costly because admitted patients are likely to be more treatment-resistant, prone to readmission, and in need of individualized care and supervision.
Reduced service for mood, anxiety and substance use disorders is also concerning because the rates of these problems increased in the general population during the pandemic.3,4,35,36 Perhaps patients found psychiatric support through virtual health care;37–39 a sharp increase in demand for virtual mental health care services, without a corresponding increase in resources, has affected service recipients and providers alike.40
The increased proportion of patients with psychotic disorders during restrictions aligns with previous work11,13,16 and extends evidence to a longer postrestriction period. Similarly, we extended evidence of increased involuntary admissions6,9,13,15,16 to a longer postrestriction period and used more equivalent comparison periods. We included a large sample encompassing nonforensic admissions to 8 Ontario psychiatric hospitals. We used the RAI–MH, a standardized and well-validated assessment tool used in hospitals across Canada (and internationally25), which enhanced the potential for the generalizability of our findings to other psychiatric hospitals in Ontario and elsewhere.
Aggression against hospital staff is associated with trauma among psychiatric workers,34 compounding pandemic-related stressors. Consequently, there is a growing need to support psychiatric health care workers by assessing patients’ violence risk and developing protocols.41 Mental health supports such as evidence-based and trauma-informed debriefing, and psychologic assessment and treatment for staff experiencing trauma, anxiety and depression are warranted.42
Future research should investigate multiple admissions and admissions not associated with an Ontario health insurance number, which likely indicate underrepresented groups. Research into the impact of the COVID-19 pandemic on forensic psychiatric services is warranted and may inform understanding of the increase in involuntary admissions. Research is also needed to determine workforce planning and development in light of the apparent postpandemic shift toward higher acuity in the psychiatric inpatient population, as well as to investigate impacts of the pandemic on patient health outcomes.
Limitations
We acknowledge there is no clear-cut definition of the COVID-19 pandemic restriction period. We conducted a secondary analysis of available, anonymized health records and excluded multiple admissions within time periods. We used a simple retrospective cross-sectional design that did not account for the nonindependence of observations across each period. Consequently, we could not examine the circumstances surrounding admissions, such as whether pandemic-related restrictions contributed. Future studies should confirm current findings using a time-series model incorporating all Ontario psychiatric hospital admissions to address these limitations.
Conclusion
Psychiatric admissions did not fully return to prerestriction levels in absolute rates and patient acuity after COVID-19 restrictions were lifted in 8 Ontario psychiatric hospitals. Given the apparent increase in clinical acuity — likely further exacerbated by the social, economic and health inequities that emerged during the pandemic — broader policy initiatives that address the social determinants of mental health and provide equitable, timely and well-coordinated access to mental health services are urgently needed. A more challenging postpandemic psychiatric inpatient population may require commensurate human resource planning and development. Organizations should analyze whether their current workforce, already challenged by the pressures of the pandemic, can meet the ongoing needs of the inpatient population and determine the steps to meet future staffing needs. These steps may involve training more staff in evidence-based guidelines for psychosis and supporting the development of skill sets needed to care for iller and more disturbed patients.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
Contributors: Elke Ham, Zoe Hilton and Soyeon Kim conceptualized and designed the study. Soyeon Kim acquired the data, and Elke Ham analyzed the data. Elke Ham drafted the manuscript, and Zoe Hilton, Jennifer Crawford and Soyeon Kim revised it critically for important intellectual content. All authors interpreted the data, approved the final version to be published and agreed to be responsible for all aspects of the work.
Funding: This study did not involve external funding sources.
Data sharing: The third-party data on which this study is based (i.e., the Ontario Mental Health Reporting System) are available to others on request at https://www.cihi.ca/en/ontariomental-health-reporting-system-metadata. Data are not available from the authors.
Supplemental information: For reviewer comments and the original submission of this manuscript, please see www.cmajopen.ca/content/11/5/E988/suppl/DC1.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/
References
- © 2023 CMA Impact Inc. or its licensors