Abstract
Background: In 2018, hospitals were mandated to record homelessness using International Statistical Classification of Diseases and Related Health Problems, 10th Revision, Canada (ICD-10-CA code Z59.0). We sought to answer whether the coding mandate affected the volume of patients identified as experiencing homelessness in acute inpatient hospitalizations and if there was any geographic variation.
Methods: We conducted a serial cross-sectional study describing 6 fiscal years (2015/16 to 2020/21) of hospital administrative data from the Hospital Morbidity Database. We reported frequencies and percentages of hospitalizations with a Z59.0 diagnostic code and disaggregated by several types of Canadian geographies. Controlling for fiscal quarter (coded Q1 to Q4) and province or territory, adjusted logistic regression models quantified the odds of Z59.0 being coded during hospital stays.
Results: The frequency and percentage of people experiencing homelessness in hospitalization records across Canada increased from 6934 (0.12%) in 2015/16 to 21 529 (0.41%) in 2020/21. Trends varied by province and territory. Recording of the Z59.0 code increased following the mandate (adjusted odds ratio 2.29, 95% confidence interval 2.25–2.32), relative to the pre-mandate period.
Interpretation: The 2018 coding mandate coincided with an increase in the use of the Z59.0 code to document homelessness in health care administrative data; however, trends varied by jurisdiction. The ICD-10-CA code Z59.0 presents a promising opportunity for standardized and routinely collected data to identify people experiencing homelessness in hospital administrative data.
People experiencing homelessness have an elevated need for health services because of high rates of chronic disease, comorbidity, substance use and mental illness, largely driven and exacerbated by poor living conditions.1–3 These living conditions also contribute to increased vulnerability to infectious diseases such as influenza, tuberculosis and COVID-19.4 Consequently, people experiencing homelessness, particularly those for whom homelessness is chronic, in particular, have comparatively high rates of hospital-based health care.4,5–7 Given the unique challenges in engaging people experiencing homelessness in research8 and the limited nature of point-in-time counts,9,10 it is difficult to evaluate interventions aimed at improving health care and health outcomes for this population. Data collected routinely during health care (i.e., health administrative data) could help fill some of this data gap as these data are readily available, cost-effective, protected through existing policies and procedures, and can be linked and monitored over time.11
The International Statistical Classification of Diseases and Related Health Problems, 10th Revision, Canada (ICD-10-CA), adapted by the Canadian Institute for Health Information (CIHI), is the Canadian standard for systematic recording of diagnoses and conditions that represent risk factors to health, such as occupational and environmental factors, and lifestyle and psychosocial circumstances.12 The ICD-10-CA codes Z55.0–65.0 capture the social determinants of health, with Z59.0 capturing homelessness status. To improve data capture of this population, it became mandatory in April 2018 to record Z59.0 when noted on routine review of the patient record.12
This directive has the potential to increase the consistency of identification of people experiencing homelessness in hospital data, which can, in turn, be used to improve understanding of how this population interacts with health care services and allow for the evaluation of policies and programs aimed at improving the health of and care for people experiencing homelessness.
We sought to describe the use of the Z59.0 diagnosis code for homelessness in Canada before and after the coding mandate. Specifically, we sought to describe the difference in the use of this code applied to acute inpatient hospitalizations between the fiscal years 2015/16 and 2020/21. We looked nationally and across jurisdictions within Canada.
Methods
Study design and setting
We conducted a serial cross-sectional descriptive study using 6 years of Canadian health administrative data housed at CIHI. To describe the difference in hospital coding for people experiencing homelessness, we chose to observe 3 years before and after the 2018 mandate to have sufficient data to quantify this difference.
In consultation with the provinces and territories, CIHI maintains the Canadian Coding Standards, which are regularly revised to keep pace with changing health care models, advancements in health care and technology, and health care information needs.12 These coding standards, including the requirement to code Z59.0 as of 2018, apply to data submitted to the Discharge Abstract Database (DAD) and the National Ambulatory Care Reporting System (NACRS). These databases are managed by CIHI and capture information about inpatient and ambulatory care encounters. In preparing hospital data for submission to CIHI, a health information professional, sometimes referred to as a hospital coder, reviews a patient’s record and assigns ICD-10-CA codes to the data that will be submitted. The coding process occurs after the patient has been discharged. For an inpatient hospitalization, the coder conducts a routine review, which generally includes reviewing the discharge summary. Depending on the hospital’s processes, the coder may review parts of the record such as notes from other health professionals who interacted with the patient.
To support compliance with the mandatory coding of Z59.0, CIHI updated the documents that are used as reference material by coders, such as the Canadian Coding Standards manual, the DAD Abstracting Manual and the NACRS Abstracting Manual. When the mandate was implemented, CIHI communicated to hospital stakeholders via electronic newsletters and held virtual education sessions on what changed in the coding standards as of April 2018. Physicians working in hospitals generally do not perform the assignment of ICD-10-CA codes and were not a target audience for these communications. However, physicians are well positioned to contribute to more consistent coding of Z59.0 through social needs screening and documentation of homelessness in their clinical notes in the patient record. A recent systematic review documented growing support for social needs screening on the part of both physicians and patients in hospital settings.13 Coders can only assign codes based on information available in the patient record.
Data sources
This analysis included 6 fiscal years (2015/16 to 2020/21) of data from the Hospital Morbidity Database (HMDB). The HMDB captures pan-Canadian administrative, clinical and demographic information on hospital discharges from acute care facilities. Inpatient and day surgery data from Quebec is submitted directly to CIHI by the Ministère de la Santé et des Services sociaux du Québec. These data are appended to CIHI’s DAD to create the HMDB.
For the HMDB, the unit of analysis was unique episodes of care, which we refer to as hospitalizations. This approach consolidates adjacent acute inpatient hospital admissions and day procedure visits, which avoids counting transfers as separate hospitalizations. As most indicators produced by CIHI use episode of care as the unit of analysis, the general methodology of episode building is published elsewhere.14 We excluded hospital records without a valid health card number, and those missing admission or discharge dates or times as their episode sequence is not traceable.
Definitions
We classified patients as homeless if the ICD-10-CA code Z59.0 was recorded in any diagnostic code attached to their record. The Canadian Coding Standards manual cites a definition from the Canadian Observatory on Homelessness that “homelessness encompasses a range of physical living situations,” including living on the streets or in places not intended for human habitation (e.g., sidewalks, parks, cars), staying in overnight shelters and staying in temporary accommodations (e.g., motels, rooming houses, with friends or family, couch surfing, temporary housing for immigrants and refugees during settlement).12,15
We identified 3 distinct time periods that have perceived relevance for coding Z59.0, namely pre-mandate (2015/16 to 2017/18), post-mandate (2018/19 to 2019/20) and late post-mandate (2020/21). Note that, as these periods are assigned by fiscal year, the first day of the 2020/21 fiscal year began on Apr. 1, 2020, and closely aligned to the start of the COVID-19-related public health measures in Canada. We distinguished between the late post-mandate period and the post-mandate period in an attempt to separate out the impacts of the pandemic that might have confounded the relationship between the 2018 coding mandate and hospital coding practices for homelessness.
In addition, we examined coding patterns by fiscal quarter or 3-month period, which approximates the division of seasons. The fiscal quarters are numbered 1 through 4, with quarter 1 (Q1) from April to June, quarter 2 (Q2) from July to September, quarter 3 (Q3) from October to December and quarter 4 (Q4) from January to March of the following calendar year. Finally, we used a dummy variable for Q1 2020 to account for the sudden decrease in overall hospitalizations that was observed during the start of the COVID-19 pandemic.16
Statistical analysis
We calculated annual frequencies and percentage of total hospitalizations with a Z59.0 diagnostic code for 2015/16 to 2020/21. We disaggregated results by province or territory, and by group of census subdivisions (CSD) based on the Statistical Area Classification (SAC) developed by Statistics Canada. These categories included major census metropolitan areas (CMAs) (Toronto, Montréal and Vancouver), all other CMAs, census agglomerations (CAs) and rural areas (non-CMA or CAs). Definitions of the SAC system can be found elsewhere.17
Logistic regression models quantified the odds of identifying people experiencing homelessness among hospital stays based on the 3 distinct time periods, using the pre-mandate period as the referent category. We calculated unadjusted, quarter-adjusted and 2 geography-adjusted models to assess which level of geography was more strongly associated with rates of Z59.0 coding. The quarter-adjusted model controlled for fiscal quarter (coded Q1 to Q4) to account for seasonality and used the Q1 2020 dummy variable to account of the sudden drop in overall hospitalizations during the start of the COVID-19 pandemic. To determine the level of geography that had the greatest impact on model effects, we created 2 models, one controlling for province or territory and the other for CSD group. Finally, we ran province- or territory-specific models, which display effect sizes by individual province or territory to illustrate differences between jurisdictions. We performed all statistical analyses using SAS version 9.4.
Ethics approval
The Canadian Institute for Health Information is an independent not-for-profit organization that has been established to collect and report on health outcomes across Canada. It is a prescribed entity under section 45 (1) of Ontario’s Personal Health Information Protection Act, allowing CIHI to hold personal health information for the purposes of compiling statistical information for the management of the health system.18 As this study used routinely collected data that was analyzed at CIHI, in accordance with their institutional privacy policies, it was exempted from research ethics approval. The views expressed in this article are the authors’ and do not necessarily represent the views of CIHI.
Results
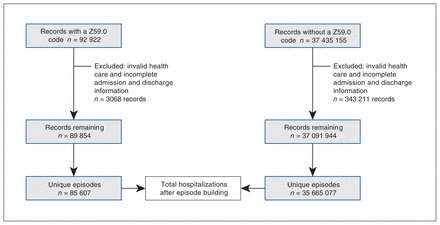
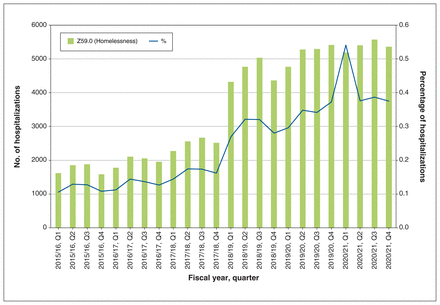
Across all years under the observation period, 85 607 (0.24%) of 35 750 684 total hospitalizations were assigned a Z59.0 diagnosis code. Over the course of episode building, 3068 (3.3%) out of 92922 Z59.0-coded records were not traceable to an episode during the entire observation period (Figure 1). The frequency and percentage of people experiencing homelessness in hospitalization records across Canada increased from 6934 (0.12%) in 2015/16 to 21 529 (0.41%) in 2020/21 (Table 1 and Figure 2; Appendix 1, Table 1, available at www.cmajopen.ca/content/11/6/E1188/suppl/DC1). The largest annual increase, 84%, occurred between 2017/18 and 2018/19.
Flow chart of Canadian hospitalization records and episode building, 2015/16 to 2020/21, from the Hospital Morbidity Database.
Frequency and percentage of hospitalizations for people experiencing homelessness by fiscal year and province or territory, 2015/16 to 2020/21*
Frequency and percentage of hospitalizations for people experiencing homelessness, as coded using the International Statistical Classification of Diseases and Related Health Problems, 10th Revision, Canada, code Z59.0, 2015/16 to 2020/21, from the Hospital Morbidity Database. Time points are displayed in fiscal quarters. For example, “2015/16, Q1” represents the period from Apr. 1, 2015, through June 30, 2015.
Provincial and territorial results
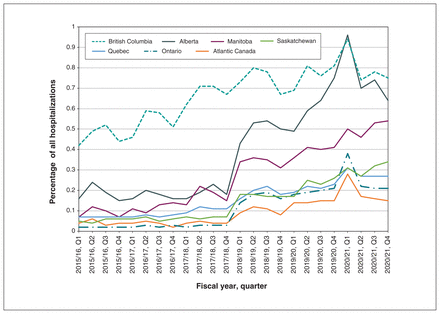
In 2020/21, facilities from 4 provinces accounted for 87% of the 21 529 recorded hospitalizations for people experiencing homelessness, namely Ontario (n = 4993, 23.2%), British Columbia (n = 6679, 31.0%), Alberta (n = 4540, 21.1%) and Quebec (n = 2546, 11.8%). From 2018/19 onward, the combined territories had the largest percentage of hospitalizations attributable to people experiencing homelessness, which was 2.2% in 2020/21. Although the hospitalizations attributed to people experiencing homelessness were relatively high in the territories, their frequencies remained small (n = 409 for 2020/21). The smallest percentage was from the combined Atlantic provinces at 0.2%. Furthermore, there was variation in coding Z59.0 across provinces and territories (Figure 3). For example, coding of Z59.0 increased in Alberta in 2018/19, whereas coding of Z59.0 in BC was proportionately more consistent throughout the observation period.
Percentage of hospitalizations for people experiencing homelessness, as coded using the International Statistical Classification of Diseases and Related Health Problems, 10th Revision, Canada, code Z59.0, by province, 2015/16 to 2020/21, from the Hospital Morbidity Database. Time points are displayed in fiscal quarters. For example, “2015/16, Q1” represents the period from Apr. 1, 2015, through June 30, 2015. Atlantic provinces (Nova Scotia, New Brunswick, Newfoundland and Labrador and Prince Edward Island) have been combined because of geographic similarities and to avoid data suppression. The territories (Northwest Territories, Nunavut, Yukon) have been removed because of small cell counts.
Census subdivision results
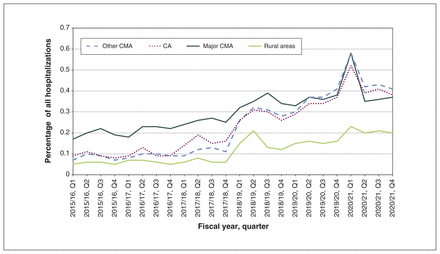
In 2020/21, facilities in major CMAs (Vancouver, Toronto, and Montréal) and other CMAs accounted for the largest percentage of the 21 529 recorded hospitalizations for people experiencing homelessness at 31.7% (n = 6828) and 45.2% (n = 9736), respectively. From 2018/19 to 2020/21, the number and percentage of hospitalizations recorded for people experiencing homelessness declined in major CMAs from 37.7% (n = 6977) to 31.7% (n = 6828) (Figure 4; Appendix 1, Table 2). However, in other CMAs and CAs, there was an increase from 40.8% (n = 7547) to 45.2% (n = 9736) and from 17.6% (n = 3264) to 19.4% (n = 4167), respectively. From 2015/16 to 2020/21, less than 5% of all recorded hospitalizations for people experiencing homelessness were from facilities in rural and remote areas.
Percentage of hospitalizations for people experiencing homelessness, as coded using the International Statistical Classification of Diseases and Related Health Problems, 10th Revision, Canada, code Z59.0, by census subdivision group, 2015/16 to 2020/21, from the Hospital Morbidity Database. For example, “2015/16, Q1” represents the period from Apr. 1, 2015, through June 30, 2015. Geographic breakdowns are based on Statistic Canada’s Statistical Area Classification. Note: CA = census agglomeration; CMA = census metropolitan areas; major CMA = Toronto, Montréal and Vancouver; other CMA = all other CMAs not classified as major; rural areas = all areas outside CMAs and CAs.
Unadjusted and adjusted odds ratios (ORs) from logistic regression models for coding of hospitalizations for people experiencing homelessness, 2015/16 to 2020/21*
Logistic regression models
Logistic regression models showed that, during both the post-mandate and late post-mandate periods, there was a significant increase in the odds of people experiencing homelessness being recorded in the hospital setting. In the unadjusted model, the odds of identification of people experiencing homelessness relative to the pre-mandate period was 2.31 (95% confidence interval [CI] 2.27–2.34) and 3.11 (95% CI 3.06–3.16) for the post-mandate and late post-mandate periods, respectively (Table 2). Further adjustment for quarter, province or territory, and CSD groups did not appreciably attenuate the effects (Table 2).
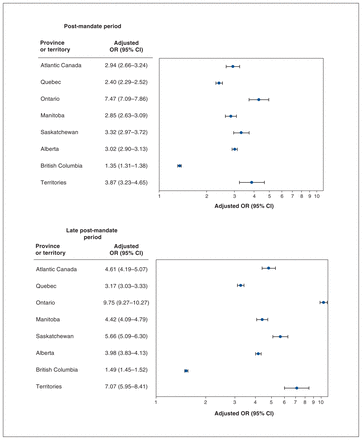
As our descriptive results of trends for Z59.0-coded hospitalizations by province or territory indicated, there was considerable variation between the provinces and territories, and the interaction between province or territory and the main effects of period proved to be significant (p < 0.001). For the models by province or territory, the highest adjusted odds ratios (ORs) were in Ontario (adjusted OR 7.47, 95% CI 7.09–7.86), the territories (adjusted OR 3.87, 95% CI 3.23–4.65) and Saskatchewan (adjusted OR 3.32, 95% CI 2.97–3.72). British Columbia exhibited the smallest increase in the odds of people experiencing homelessness being recorded in the post-mandate period (adjusted OR 1.35, 95% CI 1.31–1.38) (Figure 5), likely the result of relatively high Z59.0 coding in the years before 2018 (Figure 3).
Logistic regression models of hospitalizations coded for people experiencing homelessness in the (A) post-mandate (2018/19 to 2019/20) and (B) late post-mandate (2020/21) periods, relative to the premandate period (2015/16 to 2017/18), by province, from the Hospital Morbidity Database. All logistic regression models control for fiscal quarter (coded Q1 to Q4) and for the Q1 2020 dummy variable. Note: CI = confidence interval.
Interpretation
We examined patterns in inpatient coding of ICD-10-CA Z59.0 across Canada from 2015/16 through 2020/21. At a national level, we observed an 84% increase in coding Z59.0 following the 2018 mandate, with more than 20 000 hospitalizations in Canada coded in the 2020/21 fiscal year. We also found notable differences in coding and coding changes across provinces and territories, with some areas having only marginal increases in coding. Finally, there were proportionally more Z59.0 hospitalizations in the territories, BC and Manitoba than in Saskatchewan, Quebec, Ontario and the Atlantic provinces in the most recent fiscal year. However, absolute counts for the territories remained low, despite a large relative increase.
The significant increase in the odds of coding Z59.0 after the mandate change in 2018 was expected; however, we observed substantial variability between provinces and territories in terms of changes in Z59.0 coding. Certain areas (e.g., BC) had relatively small changes in coding volume, suggesting that some areas were already using the Z59.0 code with some regularity before the mandate, compared with other areas (e.g., Ontario, Alberta) that experienced sudden, large increases in 2018/2019. However, the change may also reflect provincial and territorial variability in concentration of urban populations, which we also found to have variable change in coding practices after the mandate was introduced.
With only 4 fiscal quarters being observed, the significant increase in the odds of coding Z59.0 during the late post-mandate period is difficult to interpret as this period coincides with the COVID-19 pandemic. However, people experiencing homelessness are known to have had a heightened infection and complication rate related to COVID-19.4,19–21 Thus, this result may be in part explained by excess COVID-19 or other pandemic-related hospital care for people experiencing homelessness. Furthermore, deferring hospital care can be more challenging for people experiencing homelessness as they have more acute needs and fewer health care alternatives than their housed counterparts.22
Despite previous research showing that homelessness is on the rise in Canada,23 it is clear that the increases we observed in 2018/2019 are at least partly due to the change to coding practices mandated in April 2018. Before 2018/19, the validity of homelessness indicators including Z59.0 was previously shown to have low sensitivity;23 however, this work was conducted before the 2018 mandate and, therefore, it is not clear to what extent the changes we observed after 2018/19 are related to coding practices as opposed to underlying changes in the population. Future research is required to validate this code after 2018/19 to understand its validity overall and between jurisdictions, which might affect its use for health system improvement and planning. In addition, further investigation into seasonal trends of hospitalizations is warranted, particularly in recent years, to better understand the societal and environmental factors that may have contributed to how people experiencing homelessness seek hospital services in the pandemic era.
Limitations
This analysis considered only people experiencing homelessness who have accessed hospital services and were documented as homeless on their medical chart by their care provider. Within or across hospitals, there may not be a systematic method for documenting residential status as part of the patient intake or assessment process. For example, those who seek shelter by couch surfing or staying with family and friends may not be considered homeless at the point of care.24 Additional ICD-10-CA codes under Z59 (i.e., Z59.1–Z59.9) capture elements of residential instability, like inadequate housing, unsuitable living conditions and extreme poverty, but these are not mandatory to code. Given this nuance, it is not known how many people experiencing homelessness remain uncaptured in hospital administrative data. People experiencing homelessness can have substantial barriers to accessing hospital care25 and have also been shown to seek care through outpatient physician clinics more than the general population.23 In addition, we included only patients with a valid health card and complete admission and discharge information, which may influence who is captured in the analysis.
The ORs that compare pre-mandate, post-mandate and late post-mandate periods make these comparisons for the average usage of Z59.0 codes in each period; the logistic regression models do not account for a secular year-on-year increase in the use of the Z59.0 code before and after the introduction of the mandate. As a result, some part of these comparisons could be attributed to this increasing secular trend. Moreover, the late post-mandate period occurred during the time of the COVID-19 pandemic and, therefore, interpretation of this period is challenging as it is unknown to what extent the increases in Z59.0 codes were the result of factors associated with the pandemic.
Conclusion
At the national level, recording of homelessness through the Z59.0 code in health care administrative data significantly increased after the 2018 coding mandate. This code has become a promising identifier that has the potential to provide a reliable source of information for health system planning and research. Future research validating the capture of this code is warranted to understand comparability between jurisdictions, generalizability of results and utility of the data for health system improvement and planning.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
Contributors: Eric De Prophetis, Kinsey Beck, Diana Ridgeway, Junior Chuang, Maegan Mazereeuw, Geoff Hynes and Keith Denny were involved in the design and conceptualization of the work. Eric De Prophetis and Kinsey Beck were involved in the analysis. Eric De Prophetis, Kinsey Beck, Diana Ridgeway, Junior Chuang, Maegan Mazereeuw, Lucie Richard and Anna Durbin were involved in the interpretation of the data. All of the authors drafted the manuscript, revised it critically for important intellectual content, gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Funding: This project was supported and funded by the Canadian Institute for Health Information.
Supplemental information: For reviewer comments and the original submission of this manuscript, please see www.cmajopen.ca/content/11/6/E1188/suppl/DC1.
Data sharing: The data that support the findings of this study are available from the Canadian Institute for Health Information (CIHI), but legislative restrictions apply to the availability of this data and data are therefore not publicly available. Permissions to access the relevant data for this study can be made through a formal request to CIHI.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/
References
- © 2023 CMA Impact Inc. or its licensors